What is Preventing Therapist Burnout
?
Everything you need to know
Taking Care of the Caregiver: A Guide to Preventing Therapist Burnout
Hello! If you’re currently in therapy, you know how much emotional energy and presence your therapist brings to every single session. They sit with your pain, celebrate your victories, navigate complex feelings, and maintain a safe, consistent space for you to heal. It’s a demanding, high-stakes job—and it relies entirely on the therapist being emotionally available and well.
Just like anyone in a deeply relational and emotionally taxing profession (nurses, teachers, social workers), therapists can experience burnout.
Burnout isn’t just “being tired.” It’s a specific kind of emotional exhaustion that leads to cynicism, detachment, and a reduced sense of personal accomplishment. When a therapist experiences burnout, it doesn’t just hurt them; it can affect the quality of care they offer you. A therapist who is burned out can’t show up fully, which means your therapeutic journey might slow down or become less effective.
It’s completely okay—and even helpful—for you, as a client, to understand this reality. Your therapist is a human being with their own finite energy resources.
Time to feel better. Find a mental, physical health expert that works for you.
This article is for you, the everyday “therapy customer.” We’re going to explore the signs, causes, and most importantly, the prevention strategies for therapist burnout. Understanding this helps you appreciate the commitment your therapist makes and gives you a compassionate lens through which to view the therapeutic relationship.
What Exactly is Burnout? Recognizing the Three Dimensions
The term burnout gained traction decades ago to describe exhaustion and low morale in demanding, helping professions. It’s officially recognized by the World Health Organization (WHO) as an occupational phenomenon defined by three key dimensions:
- Emotional Exhaustion
This is the feeling of being utterly drained, depleted, and unable to summon the emotional or physical energy to face another day of work. For a therapist, this means feeling like they have nothing left to give their clients. They feel emotionally empty, sometimes struggling to find the energy to even fake a smile or provide a genuine empathetic response. This state of persistent fatigue is often what first signals a problem.
- Depersonalization (Cynicism and Detachment)
This is a shift toward a detached, cynical, or indifferent attitude toward one’s job and the people they serve. It is a defense mechanism. Instead of feeling the empathy required for effective therapy, the burned-out therapist might start viewing clients impersonally, or mentally labeling them and their problems. They might pull back emotionally, using a veneer of technical professionalism to avoid deeper connection, which is exhausting to maintain.
- Reduced Personal Accomplishment
This is a feeling of professional inadequacy and a tendency to evaluate one’s work negatively, regardless of actual success. Even when clients are successful, the therapist feels ineffective, or feels that their efforts don’t make a significant difference. This dimension directly impacts motivation and confidence, leading to a sense of meaninglessness in the work.
A Related Concept: Compassion Fatigue and Secondary Trauma
While closely related to burnout, Compassion Fatigue is a specific, often more acute, form of secondary trauma often seen in caregiving professionals.
- Burnout results from long-term, cumulative work stress and feeling overwhelmed by workload, long hours, and organizational demands. It’s like stress from the job structure itself.
- Compassion Fatigue is the emotional, physical, and spiritual distress that results from constant exposure to the suffering and trauma of others. It’s the stress from the content of the work.
Therapists, particularly those working with severe trauma (PTSD, complex grief, abuse), are highly susceptible to compassion fatigue. It makes the world feel unsafe and can cause the therapist to experience symptoms similar to those of their clients (e.g., anxiety, intrusive thoughts, hypervigilance, difficulty sleeping, or increased irritability). Preventing burnout involves proactively managing both general work stress and the specific emotional toll of bearing witness to trauma.
The Causes: Why Therapists Burn Out
Why are therapists, who are experts in emotional health, so prone to burnout? The causes are usually multi-layered, combining systemic issues with the unique demands of the job.
- The Emotional Load (The Contagion of Pain)
Every session requires the therapist to engage in active listening, empathetic resonance, and emotional containment. They absorb, witness, and process intense, often dark, emotional material from multiple clients every day. This is emotionally draining, like using a sponge that needs regular, thorough wringing out. Furthermore, there is a concept called emotional contagion, where the therapist’s nervous system can unconsciously mirror the distress of the client
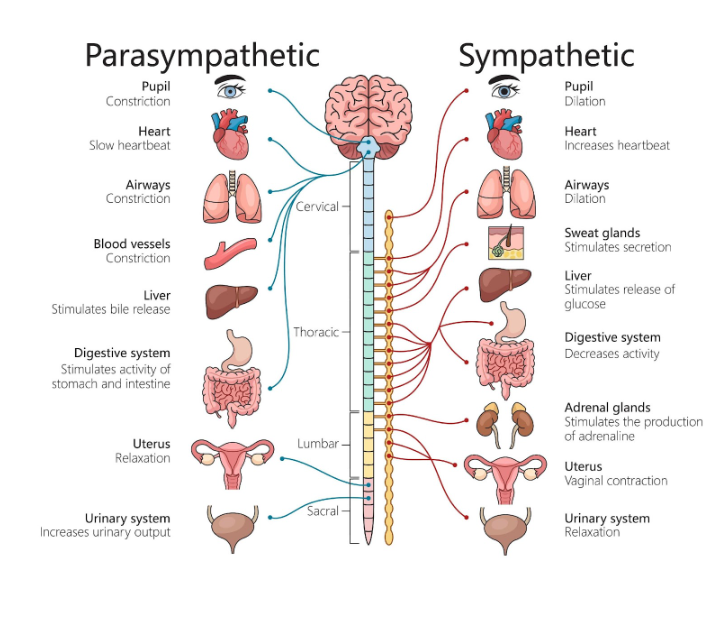
This constant need for regulation is exhausting.
- High Empathy and Boundary Challenges
Therapists rely on their capacity for empathy, but deep empathy, when unregulated, is exhausting. If a therapist doesn’t maintain strong, clear professional boundaries, they risk taking on their clients’ problems as their own. They might worry excessively about a client between sessions or feel responsible for outcomes they can’t control. Additionally, they must constantly manage their own natural human reactions—they can’t show surprise, sadness, or frustration too openly in session, which requires immense emotional regulation and suppression.
Connect Free. Improve your mental and physical health with a professional near you

- Isolation and Lack of Immediate Feedback
Unlike most office jobs, clinical therapy is often solitary work. The therapist spends their day behind closed doors, often unable to talk about the details of their work (due to confidentiality) with friends or family. They lack the immediate, positive feedback that other jobs offer (like closing a sale or finishing a project). Client progress can be slow, non-linear, and messy, making it difficult for the therapist to see the concrete, positive results of their efforts, fueling the “Reduced Personal Accomplishment” dimension of burnout.
- Organizational and Financial Stress
Many therapists, particularly those in private practice or community clinics, face significant systemic stressors:
- Administrative Burden: Dealing with insurance, billing, and mountains of complex clinical documentation (paperwork).
- Financial Pressure: Balancing the need for a sustainable income with the need to avoid overworking. This often leads to “case load creep,” where the therapist takes on too many clients to cover costs, leading to inadequate downtime between sessions.
- Lack of Breaks: Back-to-back sessions without enough time to emotionally transition means the therapist is carrying emotional residue from one client into the next.
The Warning Signs in Your Therapist
While your therapist is a professional, they are human. Recognizing subtle signs of struggle isn’t about diagnosing them; it’s about being aware of the challenges of their profession and being a supportive, compassionate participant in your shared work.
If a therapist is experiencing burnout, you might notice:
- Increased Detachment: They seem less emotionally present, less engaged in the session, or rely more on standard, canned questions rather than spontaneous, tailored responses. They might seem preoccupied.
- Increased Cynicism: They may use overly clinical, jargon-heavy language, or subtly express hopelessness about the therapeutic process (though professionalism usually prevents overt complaints).
- Scheduling Issues: They may start canceling sessions more frequently, changing appointment times often, or showing up late, indicating difficulties with personal organization and workload management.
- Difficulty Recalling Details: They might struggle to remember key facts or intimate details from previous sessions, indicating severe mental and emotional overload and reduced ability to retain information.
- Focus on the Clock: They might end sessions abruptly or seem overly concerned with the time, indicating an eager desire for the session to be over, rather than allowing the session to end naturally.
If you ever have a concern that your therapist is struggling, the most important step is to bring it up gently in session. A good therapist should be able to hear this feedback and address it professionally, perhaps by sharing that they are adjusting their schedule or even referring you to a colleague if they recognize they can’t meet your needs at that time.
Prevention and Self-Care: How Therapists Stay Well
Because burnout and compassion fatigue are occupational hazards, therapists are ethically and professionally required to prioritize their own self-care. Here are the core strategies they use, which are often the same ones they recommend to you!
- The Non-Negotiable: Consultation and Supervision
This is arguably the most vital tool and is a required component of practice. Therapists regularly meet with a clinical supervisor or a peer consultation group to discuss challenging cases, ethical dilemmas, and their own intense reactions to client material.
- The Benefit: Supervision provides an essential, confidential space for the therapist to “wring out the sponge.” They can safely process the heavy material they’ve absorbed, receive objective feedback, and ensure their professional boundaries are intact, thus mitigating compassion fatigue.
- Strict Boundary Management
High-quality therapy depends on strong professional boundaries. Therapists protect themselves by:
- Limiting Caseload: Not overloading their schedule, ensuring they have adequate breaks (at least 15 minutes) between sessions to emotionally reset, document, and transition their attention.
- Defining Work Hours: Sticking to defined start and end times, and avoiding reading emails or charting late into the evening or on weekends.
- Setting Financial Boundaries: Charging appropriate fees and managing administrative demands efficiently to ensure they aren’t forced to overwork just to survive financially.
- Personal Therapy
It is common, and often ethically encouraged, for therapists to engage in their own personal therapy when needed, or throughout their career.
- The Benefit: Personal therapy ensures the therapist addresses their own unresolved issues, preventing their own “stuff” from unconsciously interfering with a client’s process (countertransference). It’s also where they safely process the indirect stress and emotional residue of the job without burdening friends or family.
- Self-Care as an Ethical Obligation
Therapists view self-care not as a luxury, but as a professional, ethical obligation to maintain competence. This includes:
- Physical Health: Prioritizing consistent sleep, healthy nutrition, and regular exercise, which are foundational for emotional and cognitive resilience.
- Mindfulness and Grounding: Using mindfulness, meditation, or grounding techniques (like focusing on sensory input or deep breathing) to transition between clients and leave the emotional energy of the previous session behind.
- Protected Downtime: Engaging in non-work activities that bring joy, connection, and intellectual stimulation (hobbies, nature, time with loved ones, reading non-clinical books).
Your Role: A Compassionate Perspective
As a client, you might wonder if you contribute to your therapist’s burnout. The simple answer is no. Your pain is real, and the therapeutic space is designed to contain it. You should never feel pressured to minimize your struggles to protect your therapist.
However, having a compassionate understanding of the demands of their job can subtly enhance your therapeutic experience:
- Respecting Boundaries: Understand that your therapist cannot text or email with you between sessions unless it’s for administrative reasons. They need this protected, off-the-clock time to maintain their energy and focus.
- Focus on Yourself: Use the session time efficiently to focus on your own growth. You don’t need to ask them personal questions or worry about their life.
- Openness to Feedback: Be open if your therapist suggests a break, a change in schedule, or a referral. This is a sign of their professionalism and ethical commitment to you, not a rejection. It means they are responsibly managing their capacity to provide you with the best possible care.
Ultimately, preventing burnout is about recognizing the inherent humanity and limitations of the caregiving role. By understanding the effort your therapist puts into their own self-care, you can trust that they are committed to showing up as their best, most present, and most effective self for you.

Free consultations. Connect free with local health professionals near you.
Conclusion
Part 1: Detailed Guide to Therapist Burnout and Prevention Strategies
Hello! As a therapy customer, understanding the demands placed on your therapist is not just interesting—it’s crucial for appreciating the commitment they make to your well-being. The therapeutic profession is deeply rewarding, but it is also an emotionally taxing job that carries a high risk of burnout.
Burnout is a specific occupational syndrome that can compromise a therapist’s effectiveness and is defined by three key dimensions: Emotional Exhaustion, Cynicism (Depersonalization), and a Reduced Sense of Personal Accomplishment.
This article explores why therapists are susceptible to this unique type of stress, the warning signs that you might notice, and the essential, ethical strategies therapists use to stay healthy and present for you.
I. The Emotional Load: Why the Work is Exhausting
Therapists are prone to burnout due to the inherent nature of sitting with human suffering every day. This stress comes from several unique professional demands:
1. The Burden of Emotional Containment
Every session requires the therapist to engage in active listening, empathetic resonance, and emotional containment. They must absorb, witness, and process intense, often heavy or traumatic, emotional material from multiple clients daily. This requires immense internal resources. Therapists often describe this as using an emotional sponge that needs constant, thorough wringing out.
2. Compassion Fatigue and Secondary Trauma
A specific danger is Compassion Fatigue, which is the emotional, physical, and spiritual distress resulting from constant exposure to the trauma of others. Therapists who work with PTSD, severe abuse, or complex grief are particularly vulnerable.

This exposure can trigger the therapist’s own stress response systems, leading to symptoms similar to those of their clients, such as anxiety, intrusive thoughts, and hypervigilance. The constant need to regulate their own nervous system while regulating the client’s is profoundly draining.
3. High Empathy and Boundary Challenges
Effective therapy relies on deep empathy. However, when empathy is unregulated, the therapist risks adopting their clients’ problems as their own. Therapists must maintain rigorous professional boundaries to protect their emotional core, but constantly navigating where the client’s pain ends and their professional role begins is itself an energy-intensive process. They must regulate their own surprise, shock, or sadness, which requires significant emotional labor.
4. Systemic and Environmental Stress
Beyond the emotional load, therapists face common workplace stressors, often exacerbated by the nature of the work:
- Isolation: Therapy is solitary. Therapists often spend their entire day behind closed doors, unable to talk about the details of their work (due to confidentiality), which can lead to social isolation and a lack of real-time peer support.
- Lack of Immediate Feedback: Client progress is slow and non-linear. Unlike other professions, there are no immediate, concrete results (like finishing a project), which can fuel the feeling of Reduced Personal Accomplishment and erode motivation.
- Administrative and Financial Burden: Many therapists, especially those in private practice, dedicate significant, unpaid time to insurance, billing, charting, and practice management, adding to the total weekly workload.
II. The Warning Signs in the Therapist
As a client, noticing subtle shifts in the therapeutic relationship can be a sign that your therapist is struggling with their own well-being. If you observe these patterns, it’s not a judgment, but a professional signal that their capacity might be temporarily compromised:
- Increased Emotional Detachment: The therapist seems less present, less emotionally engaged, or gives standardized, “canned” responses rather than tailored, spontaneous feedback.
- Difficulty Recalling Details: They struggle to remember key emotional facts or narrative details from previous sessions, indicating mental overload and an inability to fully process client information.
- Focus on the Clock: They may end sessions abruptly or seem overly eager for the session to finish, showing a desire to escape the emotional intensity of the room.
- Scheduling Issues: Frequent, non-emergency session cancellations, late arrivals, or persistent attempts to reschedule appointments.
- Subtle Cynicism: They may use overly clinical jargon or subtly express hopelessness about the treatment process or the system.
III. Ethical Prevention Strategies: How Therapists Stay Well
Because burnout is an occupational hazard, therapists have an ethical obligation to prioritize self-care to ensure they remain competent and present for their clients.
1. Clinical Supervision and Consultation (The Non-Negotiable)
This is the most critical professional tool. Therapists regularly meet with a clinical supervisor or peer consultation group. This provides a confidential, structured space to:
- “Wring out the Sponge”: Process the heavy emotional material absorbed from clients.
- Maintain Boundaries: Receive objective feedback to ensure their professional and personal boundaries are intact.
- Manage Countertransference: Explore their own emotional reactions to client material, preventing their own issues from interfering with the client’s growth.
2. Strict Boundary Management
Therapists proactively limit their exposure and manage their resources:
- Limited Caseload: Consciously keeping client numbers at a manageable level to ensure they have sufficient emotional energy for each person.
- Buffer Time: Scheduling protected breaks (at least 15 minutes) between sessions for grounding, documentation, and mental transition.
- Protected Downtime: Strictly defining work hours, avoiding emails on evenings or weekends, and ensuring time off for vacation and recovery.
3. Personal Therapy
Many therapists engage in their own therapy, both to address personal issues and to process the secondary stress of their work. This is a core commitment to professional integrity.
4. Comprehensive Self-Care
Viewing self-care as an ethical responsibility, therapists prioritize foundational health:
- Physical Health: Consistent sleep, nutrition, and exercise.
- Mindfulness and Grounding: Using intentional techniques to transition their focus and leave the emotional energy of the previous session behind before engaging with their own life.
- Protected Joy: Engaging in hobbies, nature, and relationships that are completely separate from clinical work.
Part 2: Conclusion
Conclusion
Understanding therapist burnout is vital because the quality of therapy relies entirely on the therapist’s emotional resilience and presence. Burnout is a serious occupational syndrome driven by the unique emotional load of bearing witness to suffering, coupled with systemic work stressors.
By proactively employing ethical and rigorous self-care strategies—particularly clinical supervision, strict professional boundaries, and protected downtime—therapists fulfill their commitment to their own well-being. This deliberate effort ensures they maintain the emotional availability and clinical competence required to show up as their best, most compassionate, and most effective self for you, the client.
Time to feel better. Find a mental, physical health expert that works for you.
Common FAQs
Therapist Burnout and Self-Care
What is the difference between general stress and therapist "burnout"?
Burnout is more specific and severe than general work stress. It’s defined by three core issues:
- Emotional Exhaustion: Feeling completely drained, with nothing left to give.
- Depersonalization (Cynicism): Feeling detached or indifferent toward clients and the work.
- Reduced Personal Accomplishment: Feeling ineffective, even when progress is happening.
It’s a specific occupational syndrome, not just a bad week.
Can I, as a client, cause my therapist to burn out?
No, absolutely not. You are not responsible for your therapist’s burnout. Your pain, your struggles, and your needs are real, and the therapeutic space is specifically designed to contain them.
Burnout is primarily caused by systemic and professional factors: excessive caseloads, lack of boundary management, heavy administrative burdens, and consistent exposure to trauma (which causes Compassion Fatigue). Your role is to focus on your own healing, not to manage your therapist’s emotional state.
What is "Compassion Fatigue," and how is it different from burnout?
Compassion Fatigue is a specific form of trauma stress resulting from repeated, intense exposure to the suffering and trauma of others.
- Burnout is primarily about feeling exhausted by the workload and job structure.
- Compassion Fatigue is primarily about feeling damaged or overwhelmed by the content of the work (bearing witness to trauma).
Many therapists experience a mix of both. Dealing with a high volume of severe trauma makes a therapist highly susceptible to compassion fatigue.
What is the most important tool therapists use to prevent burnout?
The most critical tool is Clinical Supervision and Peer Consultation.
This involves meeting regularly with a senior therapist or a group of colleagues to discuss challenging cases, ethical dilemmas, and their own personal reactions (countertransference) to the client material. It’s the professional and confidential space where the therapist can “wring out the emotional sponge” and ensure their boundaries and clinical approach remain intact.
Why is a therapist's "self-care" considered an ethical obligation to me?
A therapist’s ethical obligation is to provide competent and effective care. If a therapist is burned out, they cannot show up fully, be emotionally present, or make sound clinical judgments.
Therefore, prioritizing self-care (getting enough sleep, setting strict boundaries, going to their own therapy) is seen as a professional responsibility that directly maintains their capacity to serve the client ethically and effectively.
If I notice my therapist showing signs of burnout (like detachment or canceling), what should I do?
The most helpful thing you can do is bring it up gently and respectfully in session.
You might say, “I’ve noticed you seem a little less engaged lately, and I wanted to check in. I value our work, and I hope you’re taking care of yourself.” A professional therapist should be able to hear this feedback non-defensively and address it openly. They may confirm they are adjusting their schedule or supervision to manage their workload.
Why are strict boundaries (no texting between sessions, not being friends) so important for my therapist's health?
Strong boundaries are a crucial protective shield for the therapist. They ensure the therapeutic relationship remains professional and clear.
By maintaining boundaries (like not checking emails after hours or limiting contact between sessions), the therapist protects their downtime and prevents the emotional intensity of the workday from bleeding into their personal life. This allows them to fully recharge, ensuring they have the energy and clarity to be present for you during your session time.
Do therapists have their own therapy?
Yes, many do. It is common and often ethically encouraged or even required during training for therapists to engage in personal therapy.
This is essential because it allows the therapist to address their own personal or historical issues, preventing their own “stuff” from unconsciously interfering with your process. It also provides them with a safe, confidential space to process the secondary stress and emotional burden of the job.
People also ask
Q: What are the 5 C's of burnout?
A: Based on the research and in my work with clients, I’ve identified five things that actually drive burnout. I call them the 5 Cs: Conditions, Culture, Convictions, Choices, and Capacity.
Q:What is the formula for burnout?
A: For years I’ve shared the formula with my executive clients: Burnout = High Responsibility + Low Power.
Q: How to quickly reverse burnout??
A: You can combat burnout by taking time off, setting boundaries, prioritizing rest, and seeking support through self-care and professional or peer help. Simple steps like taking small breaks throughout the day, delegating tasks, and using coping skills to reduce stress can help restore balance and prevent future burnout.
Q:What jobs have the highest burnout rates?
A: Nurses lead for those with the most burnout risk, with an estimated 6.9% burnout likelihood. This role is followed closely by ER physicians at 6.6% and primary-care doctors at 6.2% odds. Child and family social workers come in at 6.0%, while teachers and EMTs round out the top five with odds between 5.4–5.6%.
NOTICE TO USERS
MindBodyToday is not intended to be a substitute for professional advice, diagnosis, medical treatment, or therapy. Always seek the advice of your physician or qualified mental health provider with any questions you may have regarding any mental health symptom or medical condition. Never disregard professional psychological or medical advice nor delay in seeking professional advice or treatment because of something you have read on MindBodyToday.
Share this article

Let us know about your needs

Quickly reach the right healthcare Pro

Message health care pros and get the help you need.
Popular Healthcare Professionals Near You
You might also like
What is Psychodynamic Therapy Principles?
, What is Psychodynamic Therapy Principles? Everything you need to know Find a Pro Digging Deeper: A Simple Guide to […]
What is Dialectical Behavior Therapy (DBT)?
, What is Dialectical Behavior Therapy (DBT) ? Everything you need to know Find a Pro Navigating the Storm: Understanding […]
What is Cognitive Behavioral Therapy (CBT)?
, What is Cognitive Behavioral Therapy (CBT) ? Everything you need to know Find a Pro Your Thoughts Are Not […]





