Healing Starts with Safety: A Simple Guide to Trauma-Informed Care (TIC)
If you’re seeking help, you’ve likely heard the word “trauma” a lot lately. Trauma is much more than just a bad event; it’s the lasting impact of that event on your nervous system, your thoughts, your emotions, and your fundamental ability to feel safe and secure in the world.
Whether you experienced a single severe event (like an accident, a natural disaster, or an assault) or long-term stressful situations (like emotional neglect, growing up with addiction or mental illness in the family, or chronic discrimination and poverty), those experiences fundamentally shaped how your brain and body respond to stress today.
And here’s the most important part: You don’t need to be diagnosed with Post-Traumatic Stress Disorder (PTSD) to benefit from a trauma-informed approach.
If you struggle with chronic anxiety, have trouble trusting people, frequently feel overwhelmed by small things, or tend to shut down or lash out when stressed, you are likely carrying the residue of past adversity. Your body is still operating in a state of high alert, interpreting present-day triggers as past dangers.
This is where Trauma-Informed Care (TIC) comes in.
Time to feel better. Find a mental, physical health expert that works for you.
Trauma-Informed Care is not a specific type of therapy (like CBT or EMDR); it’s a fundamental shift in perspective for all caregivers, from your therapist to your doctor to the staff at a community center. It asks one crucial, compassionate question: “Instead of asking, ‘What is wrong with this person?’ let’s ask, ‘What has happened to this person?'”
It moves the focus from symptoms and pathology (what is broken) to safety, resilience, and healing (what can be restored). It recognizes that healing cannot happen until a person feels secure, respected, and in control.
This article is your warm, supportive guide to understanding the principles of Trauma-Informed Care. We’ll show you why this approach is so empowering, how it changes the therapy room, and what you should look for to ensure your healing journey is as safe and supportive as possible.
Part I: Understanding the Lens of Trauma-Informed Care
To truly grasp TIC, we need to understand how trauma fundamentally impacts the body and mind, which is often a biological response.
- Trauma is a Biological Event, Not Just a Memory
Trauma is stored in the body’s nervous system, not just the logical, narrative part of the brain. When a terrifying event happens, the rational brain (the prefrontal cortex, the part that uses language and planning) often shuts down, and the survival brain (the amygdala and brainstem) takes over.
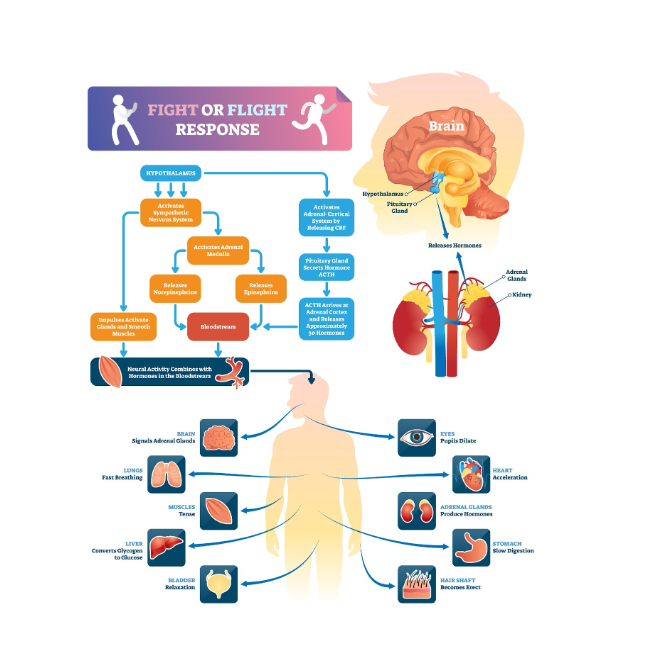
- Survival Mode: This survival brain only knows how to activate the survival responses: fight, flight, or freeze.
- The Residue: If you couldn’t complete the survival response (for example, if you wanted to fight back but couldn’t, or you couldn’t run away and had to freeze), that intense, defensive energy gets trapped in the nervous system. This trapped energy is what makes you feel hyper-vigilant, jumpy, panicked, or numb years later—even when you are objectively safe. Your body is still trying to finish the fight or flight it couldn’t complete.
- The Shift from “What’s Wrong?” to “What Happened?”
The core philosophy of TIC is empathy and non-judgment. It transforms the way challenging behaviors are viewed.
- The Old Approach (Pathology): If a client is constantly missing appointments, yelling at staff, or acting impulsively, an old-school approach might label them as “unmotivated,” “non-compliant,” “borderline,” or “difficult.” This approach focuses on diagnosing and correcting flaws.
- The TIC Approach (Context): A trauma-informed professional looks at those same behaviors and asks: “Is this client missing appointments because they struggle to trust institutional settings after a past abuse experience? Is the yelling a fight response because they feel unsafe or unheard? Is the impulsivity a need to flee an intense, unbearable feeling?”
This shift instantly re-frames a “problem person” into a “person with a wound” using an understandable survival strategy. It changes the goal from controlling behavior to supporting the need for felt safety and teaching new, effective coping skills.
Part II: The Four R’s and Six Key Principles
The U.S. Substance Abuse and Mental Health Services Administration (SAMHSA) outlines four core assumptions (the 4 R’s) and six guiding principles for TIC. These principles are the standards your caregivers should be meeting to ensure a truly trauma-informed environment.
The Four R’s: The TIC Assumptions
- Realize: All people involved in the organization (therapists, doctors, nurses, administrators) realize the widespread impact of trauma and understand the potential paths for healing and recovery.
- Recognize: They recognize the signs and symptoms of trauma in clients, family members, staff, and others involved.
- Respond: They integrate that knowledge and respond by putting TIC principles into practice in all interactions.
- Resist Re-Traumatization: They actively work to resist re-traumatization in their practices and procedures (e.g., avoiding sudden loud noises, forced physical touch, or unexpected changes in routine without warning).
The Six Guiding Principles: What You Should Experience
These principles define what a safe, trauma-informed environment feels like for you and are a great checklist when looking for a provider:
- Safety (Physical and Emotional)
This is the non-negotiable first step. The environment must feel physically safe (well-lit, clean, calm) and, more importantly, emotionally safe.
- In Practice: A trauma-informed therapist is highly predictable and consistent. They keep the same schedule, they have clear and consistent professional boundaries, and they are emotionally regulated themselves. They ask before starting an intense discussion, ensuring you feel ready and resourced enough to handle the material.
- Trustworthiness and Transparency
Trust is the foundation of healing and is rebuilt through consistent, clear communication and reliability.
- In Practice: Your therapist should be transparent about fees, cancellations, confidentiality limits, and what they write in your session notes. They explain the therapeutic plan and your role clearly. There are no hidden agendas, sudden rule changes, or vague processes.
- Peer Support
Incorporating the lived experience of people who have already gone through healing can be hugely empowering, reducing feelings of isolation and shame.
- In Practice: This might mean recommending group therapy led by peers, or simply the therapist sharing general stories of hope and recovery from other clients (always maintaining strict confidentiality and anonymity).
- Collaboration and Mutuality
Decisions about your care are made with you, not to you. The power imbalance that exists between client and professional is minimized and actively managed.
- In Practice: You have a voice in choosing the type of therapy, the speed of the sessions, and what topics you address each week. The therapist acts as a partner, sharing knowledge and expertise, but respecting you as the ultimate authority on your own life.
- Empowerment, Voice, and Choice
Trauma often involves having your sense of control violently taken away. Healing requires giving that control back.
- In Practice: The therapist gives you choices constantly about small things: “Would you like the door open or closed?” “Would you rather talk about the past or stick to coping skills today?” “We could work on this memory, but we can stop at any time you feel overwhelmed.” This continuous offering of control prevents re-traumatization.
- Cultural, Historical, and Gender Issues Competence
The approach must honor your cultural background and understand the trauma that specific groups (e.g., marginalized communities, LGBTQ+ individuals, people of color, refugees) may experience due to systemic issues like racism, sexism, or discrimination.
- In Practice: Your therapist understands that a client of color may experience hyper-vigilance not just because of personal family history, but because of real, ongoing, systemic threats. They recognize that healing requires acknowledging the societal context of pain, not just the individual context.
Connect Free. Improve your mental and physical health with a professional near you

Part III: What TIC Looks Like in Your Therapy Room
How do these principles translate into the actual practice of a trauma-informed therapist?
- Pacing and Titration
A trauma-informed therapist knows that forcing emotional processing too quickly is re-traumatizing.
- Titration: This means working in small, tolerable doses. If you are discussing a difficult memory, the therapist might stop you, ask you to take a breath, focus on a neutral object in the room (like a plant or a piece of art), and check your body sensations before proceeding. They keep the dosage of difficult material small enough for your nervous system to handle without being overwhelmed or triggering a shutdown.
- The Container: They help you establish mental resources and safety, like a “Safe Place” visualization or a “Container” visualization to metaphorically store overwhelming material until you are ready to address it.
- Prioritizing Regulation Over Insight
The therapist focuses on calming your nervous system before trying to understand why you are upset.
- First, Grounding: If you enter the room feeling panicked, activated, or disconnected, the therapist won’t immediately ask, “What are you thinking?” or “What’s the meaning of this feeling?” They will first engage in grounding techniques: “Let’s put your feet flat on the floor, feel the chair under you, and notice five things you can see.” This technique brings your survival brain offline and into the present moment, which is the only state in which true healing and insight can occur.
- Somatic Awareness: They help you notice the bodily sensations associated with emotion (“Where do you feel that anxiety in your body? Is it tight? Warm?”). This helps you connect the mind and body and track when you are moving into distress, giving you crucial seconds to choose a coping skill.
- Language of Non-Pathology
A trauma-informed therapist uses language that validates your struggle and survival attempts rather than pathologizing or judging them.
Language of Pathology (Judgment) | Trauma-Informed Language (Compassion) |
|---|---|
“You are being non-compliant.” | “We need to address your difficulty following through. I wonder if there is fear involved.” |
“You need to control your anger.” | “You are having a survival response. Let’s find a safer way to discharge that energy.” |
“You are resistant to change.” | “It makes sense that you feel hesitant. We can slow down until you feel safer and ready.” |
“You are addicted to drama.” | “It sounds like you were conditioned to feel safe only when things were intense. Let’s find stability.” |
Conclusion: You Deserve Safety and Control
Trauma-Informed Care is a commitment from your professional to recognize the profound and often unseen impact of your past. It ensures that the very environment intended to heal you doesn’t accidentally wound you again.
By understanding the principles of TIC—especially safety, choice, and collaboration—you are empowered to choose caregivers who honor your history and prioritize your stability. Healing is possible, and the journey begins when you know, without a doubt, that you are truly safe and in control of your own process.

Free consultations. Connect free with local health professionals near you.
Conclusion
Sustaining Safety, Choice, and Empowerment in Your Healing Journey
You’ve explored the fundamental principles of Trauma-Informed Care (TIC), recognizing that it is not a specific type of therapy, but a comprehensive shift in perspective guided by the question: “What has happened to this person?” You now understand that TIC is built upon recognizing the widespread impact of trauma, avoiding re-traumatization, and upholding the six guiding principles: Safety, Trustworthiness, Peer Support, Collaboration, Empowerment, and Cultural Competence.
This concluding article focuses on integration and self-advocacy: how to sustain the safety and empowerment gained from working with a trauma-informed provider and ensure that you remain the author of your own healing story. The goal is to move from being a recipient of care to being an informed partner in your long-term wellness.
Phase 1: Internalizing the Trauma-Informed Lens
The most powerful long-term shift you can make is internalizing the compassionate, non-judgmental lens of TIC and applying it to yourself.
- Reframing Your Own Behavior
TIC teaches us to view challenging behaviors as survival strategies. When you experience intense emotions, anxiety spikes, or relational conflicts, pause and apply the “What Happened?” filter to yourself.
- Self-Compassion, Not Blame: If you cancel an appointment last minute, instead of criticizing yourself (“I’m lazy and non-compliant”), use the TIC reframing: “My body is feeling deeply unsafe right now, and cancelling was a flight response to protect myself from an unknown emotional threat.” This shift replaces shame with curiosity, which is the necessary doorway to self-regulation.
- Valuing Survival: Acknowledge that the coping mechanisms you developed (e.g., people-pleasing, shutting down, hyper-vigilance) were intelligent survival tools that protected you during the trauma. They aren’t flaws; they are historical strategies. This internal validation is the opposite of the invalidation often experienced in the past.
- Prioritizing Regulation First
Your trauma-informed therapist prioritized calming your nervous system before seeking intellectual insight. You must continue this practice in daily life.
- Mindfulness of Activation: Learn to recognize the subtle physical cues that indicate your survival brain is taking over—a tightening in the stomach, shallow breathing, racing thoughts, or sudden heaviness in the limbs.
- Immediate Grounding: When activation begins, immediately deploy a simple grounding technique (like the 5-4-3-2-1 technique or deep belly breathing) before attempting to talk or problem-solve. Trying to use logic when the survival brain is screaming is ineffective. Regulation must precede reflection.
Phase 2: Sustaining Safety and Choice in All Environments
The principles of TIC should extend beyond the therapy room and influence your decisions about jobs, relationships, and even where you spend your time.
- Upholding Your Need for Choice and Voice
Trauma survivors often struggle to assert boundaries because of the fear of conflict or abandonment. Sustaining empowerment means continually exercising your voice and choice, even in small matters.
- Relational Boundaries: In relationships, consciously give yourself the right to choose the pace and direction of intimacy and vulnerability. If a friend asks for something you don’t feel ready to give, assert your boundary: “I can’t commit to that right now, but I appreciate you asking me.” Every time you choose your boundary, you reinforce the message that your autonomy is intact.
- Creating a Safe Home Environment: Actively organize your living space to support your nervous system. This means controlling the environmental factors that trigger a stress response: controlling noise levels, ensuring clear escape routes (not sitting with your back to the door), and maintaining organizational predictability (Trustworthiness).
- The Power of Collaboration (Self-Advocacy)
You are the expert on your own life. Sustaining an empowered mindset means confidently engaging with all healthcare providers (doctors, dentists, specialists) using the principles of TIC.
- Asking for Transparency: Don’t hesitate to ask your doctor to be transparent: “What exactly are you doing, and why?”
- Requesting Choice: When facing a potentially invasive or stressful procedure, assert your choice: “I need to know I can stop this procedure at any point.” This simple request honors your agency and helps your nervous system remain calm during stress.
Phase 3: Long-Term Healing and Resilience
TIC establishes the safety needed for deeper, trauma-specific therapies (like EMDR, Somatic Experiencing, or trauma-focused CBT) to be successful. The conclusion of the initial trauma-informed work marks the beginning of resilience-building.
- The Integration of Pain and Strength
TIC teaches that you are more than your trauma. Your journey now involves integrating the painful history with your present strength.
- Moving from Victim to Survivor: This shift is marked by recognizing that the parts of you that survived—the creative, resilient, determined parts—are stronger because of what they overcame. Your sensitivity is not a flaw, but a survival skill that, once regulated, becomes the source of your empathy and connection.
- Supporting Systemic Change
Because TIC emphasizes Cultural, Historical, and Gender issues, true long-term integration often involves recognizing the broader impact of systemic trauma (racism, inequality, historical oppression).
- Community Connection: Sustaining healing often involves connecting with communities or engaging in advocacy work that addresses the root causes of trauma. This moves the focus from personal pathology to social justice, turning personal pain into collective purpose and reinforcing the principle of Peer Support.
By internalizing the principles of TIC, you leave behind the judgment and shame of the past and assume the role of your own compassionate, trustworthy caregiver. You know your rights, you know your body, and you prioritize safety and choice above all else, securing the foundation for a truly healthy and integrated future.
Time to feel better. Find a mental, physical health expert that works for you.
Common FAQs
Here are some common questions people have when exploring or seeking services rooted in Trauma-Informed Care.
What is the fundamental principle of Trauma-Informed Care (TIC)?
The fundamental principle of TIC is a shift in perspective from “What is wrong with you?” to “What has happened to you?” It assumes that a person’s difficult behaviors or symptoms are often survival strategies developed in response to past trauma or adversity.
Is Trauma-Informed Care a type of therapy, like CBT or EMDR?
No, TIC is not a specific type of therapy. It is a philosophy, a framework, or a universal approach that should guide all interactions across all settings (therapy, medical, schools, social services). A therapist can practice Trauma-Informed Care while using a specific modality like CBT, EMDR, or Psychodynamic therapy.
Do I need to have a PTSD diagnosis to benefit from TIC?
Absolutely not. TIC is beneficial for anyone who has experienced adversity, chronic stress, neglect, or relational trauma—even if they don’t meet the criteria for PTSD. If you struggle with chronic anxiety, hyper-vigilance, emotional overwhelm, or trust issues, a TIC approach will prioritize your safety and stability.
How does TIC view trauma?
TIC views trauma as a biological event that leaves a lasting impact on the body’s nervous system. Trauma is seen as uncompleted survival energy (fight, flight, or freeze) that gets trapped, causing people to react to current, safe situations as if they were still in danger.
What are the Six Guiding Principles of TIC?
These principles define what a safe, trauma-informed environment should look and feel like:
- Safety: Physical and emotional safety is prioritized.
- Trustworthiness and Transparency: Clear, consistent communication about policies and procedures.
- Peer Support: Incorporating the experience of those who have healed.
- Collaboration and Mutuality: Sharing power and making decisions with the client.
- Empowerment, Voice, and Choice: Maximizing the client’s control over their own healing process.
- Cultural, Historical, and Gender Issues Competence: Recognizing and addressing systemic sources of trauma (like discrimination).
Why is "Choice" so important in a trauma-informed setting?
Trauma often involves having one’s sense of control or agency violated. Giving the client choice (e.g., choosing the topic, the pace, or the seating arrangement) and respecting their autonomy are fundamental healing mechanisms that counteract the powerlessness experienced during the trauma.
What is "Pacing and Titration"?
This is how a TIC therapist prevents re-traumatization.
- Pacing: The therapist intentionally slows down the process and does not rush into painful material.
- Titration: The therapist only allows the client to access or experience a small, tolerable dose of emotional material at a time, ensuring the client’s nervous system can process it without becoming overwhelmed.
What should a TIC therapist do if I come into a session highly anxious or triggered?
The therapist will prioritize regulation over insight. They will first focus on calming your nervous system using grounding techniques (e.g., focusing on sensory input, breathing, or noticing the feet on the floor). They will not immediately ask you to analyze why you are upset, because true insight is only possible once the survival brain has calmed down.
How does TIC change the language used in therapy?
A TIC therapist uses language that validates and humanizes the client’s struggles, moving away from language that pathologizes. For example, they might describe a coping mechanism as a “survival strategy” instead of labeling the client as “resistant” or “non-compliant.” This fosters self-compassion.
How can I practice TIC principles for myself outside of therapy?
You can become your own trauma-informed partner by:
- Applying the “What happened?” filter to your own challenging behaviors instead of self-blame.
- Consciously choosing grounding techniques whenever you feel activated.
- Asserting your choice and voice in small daily interactions to rebuild your sense of control.
People also ask
Q: What is trauma-informed healing?
A: Trauma-informed care (TIC) is an approach based on a foundation of knowledge about trauma and the paths to treatment, a response based on that knowledge and a desire to avoid re-traumatization, according to SAMHSA. Mars Girolimon.
Q:What is the primary purpose of trauma-informed care (TIC)?
A: Trauma-Informed Intervention and Treatment Principles. TIC is an intervention and organizational approach that focuses on how trauma may affect an individual’s life and his or her response to behavioral health services from prevention through treatment.
Q: What are the 6 principles of TIC?
A: The principlesa are safety, trustworthiness and transparency, peer support, collaboration and mutuality, empowerment and choice, and humility. These principles can be used in clinical and mental health care settings, workplaces, educational institutions and other organizations.
Q:What is trauma healing?
A: Trauma healing aims to help victims cope with post-traumatic stress symptoms such as anxiety, flashbacks, insomnia, and emotional disturbances. For children, methods like play, art, and group activities are used to calm emotions, create safety, and help them express fears, manage emotions, and build self-confidence.
NOTICE TO USERS
MindBodyToday is not intended to be a substitute for professional advice, diagnosis, medical treatment, or therapy. Always seek the advice of your physician or qualified mental health provider with any questions you may have regarding any mental health symptom or medical condition. Never disregard professional psychological or medical advice nor delay in seeking professional advice or treatment because of something you have read on MindBodyToday.
Share this article

Let us know about your needs

Quickly reach the right healthcare Pro

Message health care pros and get the help you need.
Popular Healthcare Professionals Near You
You might also like
What is Face Your Fear and…
, What is Exposure Therapy for Anxiety? Everything you need to know Find a Pro Facing the Fear Monster: A […]
What is Psychodynamic Therapy Explained Guide?
, What is Psychodynamic Therapy Principles? Everything you need to know Find a Pro Digging Deeper: A Simple Guide to […]
What is DBT Therapy Made Simple…
, What is Dialectical Behavior Therapy (DBT) ? Everything you need to know Find a Pro Navigating the Storm: Understanding […]





