Healing the Whole Story: A Simple Guide to Trauma-Informed Care
Hello. If you’re exploring therapy, you’re looking for a safe place to heal. If you have experienced difficult, painful, or overwhelming events in your past—and most people have—you need a therapist who understands how those experiences might still be shaping your life today.
That’s where Trauma-Informed Care (TIC) comes in.
Trauma-Informed Care is a revolutionary approach that doesn’t just treat your symptoms (like anxiety or depression); it treats you—the whole person—by acknowledging and responding to the pervasive impact of trauma in your life. It shifts the entire focus of the healing process from correction to compassion.
Instead of asking, “What is wrong with you?” a trauma-informed professional asks, “What happened to you?”
This shift in perspective is profound. It moves away from judgment, blame, or diagnosis, and toward understanding, safety, and empowerment. It recognizes that many of the struggles you face—difficulty regulating emotions, challenges in relationships, feeling constantly on edge, or struggling with intrusive thoughts—are often normal human adaptations and survival strategies that developed in response to abnormal, difficult experiences.
Time to feel better. Find a mental, physical health expert that works for you.
This article is your supportive guide to understanding TIC. We’ll explore the core principles that define this compassionate approach, how it changes your therapy sessions, and why it’s the safest and most effective way to begin (or continue) your journey toward integrated healing.
Part 1: What is Trauma, and Why Does It Need a Special Approach?
Before defining the care, we need to understand the experience. Trauma is not just a “bad memory” or a single stressful moment. It’s a fundamental change to the way your body and mind process and respond to the world.
Defining Trauma Simply
Trauma is an emotional response to an event or series of events that you experienced as life-threatening, overwhelmingly stressful, or deeply damaging to your sense of self and safety.
The key word here is overwhelming. Trauma happens when your ability to cope, process, and integrate emotions is exceeded by the event itself. It leaves you with a lasting sense of fear and helplessness, often because the event was unpredictable, inescapable, or violated your deepest trust.
Trauma is often categorized in a few ways:
- Acute Trauma: A single, terrifying event that happened quickly (e.g., a car accident, a natural disaster, a sudden assault).
- Chronic Trauma: Repeated, prolonged, or sustained exposure to highly stressful events where escape or resolution was difficult (e.g., domestic violence, ongoing neglect, repeated bullying, living in chronic danger or poverty).
- Complex Trauma: Exposure to multiple traumatic events, often interpersonal and invasive, occurring early in life and/or within primary caregiving relationships (e.g., childhood abuse, long-term relational betrayal). This often affects the ability to form healthy attachments and regulate emotions as an adult.
How Trauma Changes the Brain and Body
When you experience trauma, your body’s built-in survival system—the amygdala (the brain’s alarm center) and the rest of the nervous system—gets stuck in the “on” position.
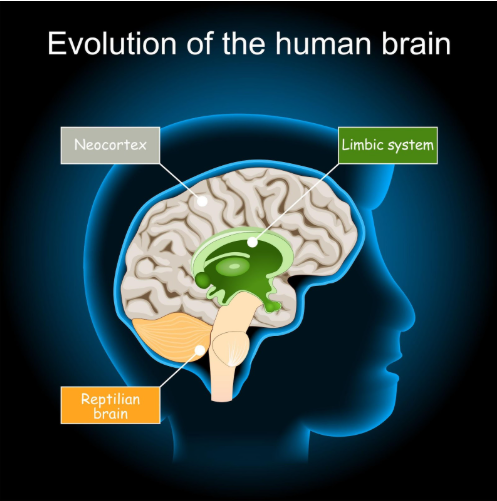
- Survival Behaviors: Many behaviors that seem problematic (like withdrawing, self-sabotaging, using substances, having intense mood swings, or avoiding intimacy) are actually protective mechanisms your brain and body developed to survive the overwhelming threat. The trauma-informed professional sees these not as flaws or signs of weakness, but as desperate, often brilliant, attempts to feel safe when no safety was present.
Part 2: The Core Shift: From “What’s Wrong?” to “What Happened?”
The entire philosophy of Trauma-Informed Care (TIC) rests on a single, vital shift in perspective. It’s moving away from a clinical, detached approach and adopting one of deep empathy and curiosity.
The Problem with the Old Approach
The old, non-informed approach often focuses only on the visible symptoms and labels them as pathologies:
- “You are aggressive and uncooperative.”
- “You can’t manage your emotions, you’re too reactive.”
- “You are non-compliant with treatment.”
This approach leads to diagnosis and medication, but often misses the underlying cause. It makes the client feel like a broken object that needs fixing, reinforcing feelings of shame and isolation. It completely fails to recognize the inherent strength required to survive trauma.
The Healing Power of the TIC Question
The TIC approach acknowledges that the person’s current behaviors are a logical, though often outdated, response to their history:
- “Why is this person struggling to feel safe and calm right now?”
- “What overwhelming experience led them to withdraw or become highly guarded?”
- “How did they learn that intense emotion was the only way to be heard or to protect themselves?”
This shift—from blame to curiosity—fosters compassion and builds the trust necessary to heal, because it validates the client’s experience rather than pathologizing it. It creates the therapeutic environment necessary for complex healing.
Part 3: The Four Pillars of Trauma-Informed Care
To make the approach practical, we can summarize the core elements into four foundational principles you should look for and expect from your trauma-informed therapist.
Connect Free. Improve your mental and physical health with a professional near you

Pillar 1: Safety (Physical and Emotional)
This is the first and most crucial element. A trauma survivor needs to feel absolutely safe in the present moment before any deep work can begin.
- Physical Safety: Your therapist ensures the physical environment is non-threatening. This means comfortable seating arrangements, clearly marked exits (so you don’t feel trapped), reliable schedules (no sudden, confusing cancellations), and predictable boundaries regarding physical space.
- Emotional Safety: This is the most important. The therapist ensures you feel validated, respected, and believed. They never push you to talk about trauma before you state you are ready. They are careful with their tone and body language, and they maintain strict, consistent confidentiality (with the required legal limits).
Pillar 2: Trustworthiness and Transparency
Trauma often involves betrayal, inconsistency, or violation from people in positions of power. The healing relationship must be the opposite: reliable and clear.
- Clear Communication: Your therapist is completely transparent about policies, fees, confidentiality limits, and their treatment plan. There are no hidden agendas or surprises. You know what to expect and when to expect it.
- Reliability: The therapist models consistency by starting and ending sessions on time, promptly returning calls or messages, and always following through on commitments. This consistency slowly teaches the nervous system that this new relationship is safe and predictable, slowly rebuilding the capacity for trust in others.
Pillar 3: Collaboration and Mutuality (Shared Power)
In trauma, power and control were often taken away. In healing, power must be shared and restored. This is a deliberate reversal of the helplessness and powerlessness often felt during the traumatic event.
- Shared Decision-Making: All major decisions about treatment goals, pace, and techniques are made together. You are seen as the expert on your own life, history, and internal experience, and the therapist is the expert on healing strategies.
- No Hierarchy: The therapist strives to eliminate the clinical hierarchy. They don’t dictate or assign; they partner and invite. They might use language like, “I have some skills that might help, but let’s test them out together to see if they feel right for your body and your history.”
Pillar 4: Empowerment, Voice, and Choice
This principle is the core of trauma recovery. It focuses on restoring the sense of agency—the ability to act on your own behalf—that trauma stripped away.
- Client Choice: The client always has the right to choose the pace, topic, and level of detail. If you want to stop talking about something, you can say, “I need to pause,” or simply put up your hand. A trauma-informed therapist will immediately respect that boundary as a vital part of your healing process.
- Focus on Strengths: The therapist deliberately focuses on your strengths and resilience—the inner resources and coping skills that helped you survive the past—rather than just cataloging your deficits. They highlight the ways you have already coped and survived, building confidence for the challenging work ahead.
- Skill Building (Resourcing): Treatment focuses heavily on resourcing—teaching you concrete skills (like grounding, emotional regulation, and self-soothing) so you feel capable and prepared to handle emotional intensity before diving into past memories.
Part 4: How TIC Changes Your Therapy Session
When you work with a trauma-informed professional, the sessions feel different, often in subtle but profound ways, because the safety of your nervous system is the priority.
- The Pacing is Slower and More Deliberate
A TIC therapist understands that rushing a client into processing trauma memories can trigger a re-traumatization—re-experiencing the event without having the resources to manage it safely.
- Stabilization First: The therapist will spend a significant amount of time in the beginning (and throughout the treatment) ensuring you are stable and regulated in the present. If a memory comes up, the therapist will help you practice the pendulum swing—the ability to look briefly at a difficult memory and then immediately swing back to a safe, positive, or neutral resource in the present moment. This teaches your nervous system that you can tolerate the feeling without being overwhelmed by it.
- Focus on the Body and Nervous System (Somatic Work)
Trauma is stored in the body’s survival responses, not just the mind’s narrative. A trauma-informed therapist pays close attention to non-verbal cues and uses somatic (body-based) techniques.
- Body Awareness: They may gently ask you, “What do you notice in your body right now?” or “Where do you feel that anxiety—is it tightness in your chest or shoulders?”
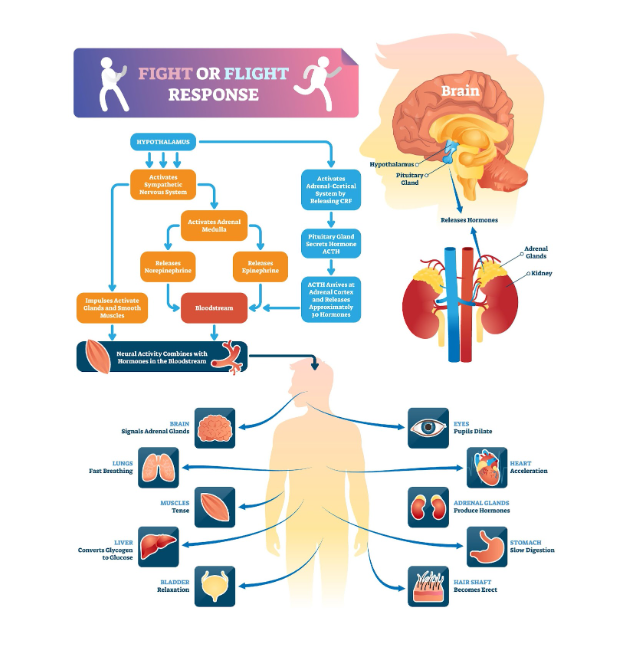
This helps you reconnect with your physical experience; which trauma often disconnects you from (dissociation or numbness).
- Grounding: The therapist teaches and utilizes grounding techniques (sensory tools like feeling your feet on the floor, focusing on five things you see, or using temperature) to bring you back to the present moment whenever you feel overwhelmed or disconnected.
- Language is Consciously Chosen and Non-Blaming
The therapist is meticulous about their language to avoid triggering feelings of shame, blame, or coercion.
- Avoid Pathologizing: Instead of saying, “You are having an irrational mood swing,” they might say, “Your nervous system is reacting to a perceived threat from the past; let’s see what skill we can use to help regulate it.”
- Emphasis on Agency: They use language of choice and invitation: “Would you be willing to try this exercise?” or “Feel free to stop me immediately if this becomes too much. I will respect your no.” They consciously avoid “You should” or “You need to,” which can feel coercive to a trauma survivor.
Part 5: The Benefits of Trauma-Informed Care
Choosing a TIC approach offers several key advantages for your healing journey:
- Increased Safety: By prioritizing emotional and physical safety, TIC minimizes the risk of re-traumatization and allows you to build trust at your own pace, creating a solid foundation for deeper work.
- Reduced Shame: By reframing “symptoms” as “survival strategies,” TIC dramatically reduces self-blame and shame, which are huge barriers to healing. It validates that your response to trauma was appropriate for the situation, even if the behaviors are no longer helpful today.
- True Empowerment: By restoring choice and control, TIC helps you reclaim your personal agency. You leave therapy not just feeling better, but feeling stronger, more competent, and more in charge of your life and emotions.
- Holistic Healing: By working with both the cognitive mind (thoughts and narrative) and the somatic body (nervous system responses and survival energy), TIC leads to more complete, integrated, and lasting recovery.
A Final Word of Warmth
If you have survived trauma, your story is a testament to incredible strength and resilience. Trauma-Informed Care honors that strength.
This approach is about creating a space where you are seen, believed, and respected. It acknowledges that your healing is not about fixing a broken person, but about gently tending to a wounded survivor and helping your nervous system realize that the danger is finally over and that a safe, stable life is possible.
By seeking out a trauma-informed professional, you are choosing the most compassionate, safe, and effective path to healing the whole story and embracing your capacity for profound recovery.

Free consultations. Connect free with local health professionals near you.
Conclusion
Reclaiming the Narrative—The Enduring Power of Trauma-Informed Healing 🫂
We have explored the revolutionary framework of Trauma-Informed Care (TIC), moving through its core philosophy, its four foundational pillars (Safety, Trustworthiness, Collaboration, and Empowerment), and its practical application in the therapy session.
The journey through TIC is ultimately about the reclamation of your life’s narrative, transforming the story from one of victimization and brokenness to one of survival and profound resilience.
The conclusion of this journey marks not a sudden endpoint, but the moment you fully integrate two vital truths: first, that your past pain was not your fault; and second, that your present struggles are not flaws, but intelligent, though now outdated, strategies your nervous system deployed to keep you alive.
From Survival Mode to Thriving: A New Nervous System Setting
The most tangible, lasting gift of TIC is the shift it creates within your own biology—specifically, in your nervous system. Trauma keeps the brain’s alarm system, the amygdala, hyper-vigilant, leading to a state of chronic stress known as hyper-arousal (fight/flight) or hypo-arousal (freeze/numbness).
- The Skill of Regulation: TIC therapy dedicates significant time to resourcing—teaching you concrete, reliable, and accessible skills (like grounding and somatic awareness) to bring your nervous system back into a state of balance. You learn to recognize the subtle physical cues of dysregulation (a tight jaw, shallow breath, a sudden urge to flee) and intervene before they spiral into a crisis.
- Expanding the Window of Tolerance: The goal is to expand your Window of Tolerance—the optimal zone where you can manage emotions, think clearly, and stay engaged in life. By safely practicing the pendulum swing (briefly touching a difficult emotion and returning to a safe resource), you teach your nervous system that intense feelings are tolerable and survivable, slowly stretching the capacity of that window. This shift means less time spent in chaos or numbness, and more time spent feeling present and capable.
Empowerment: The Core Engine of Recovery
Trauma stripped you of your voice and your choice. The ethical and clinical imperative of TIC is to restore that agency. The collaboration and empowerment principles ensure that your recovery is a co-created process where you are the ultimate authority.
- Reclaiming Autonomy: Every time a TIC therapist asks, “Would you be willing to try this?” or “We can stop at any time,” they are reinforcing your autonomy. This repeated validation—that your boundaries matter and your “no” is respected—serves as a powerful, corrective emotional experience that directly counters the helplessness of the past.
- Focus on Resilience: TIC deliberately shifts the lens away from deficits (“You have trust issues”) toward resilience (“You survived immense betrayal, which proves your incredible capacity for self-protection”). This reframing is essential because healing is not about fixing what is wrong; it is about recognizing and strengthening what is already right within you. By honoring the survival strategies, you developed, you transform shame into self-compassion.
Integration: Healing the Whole Self
TIC moves beyond treating the mind’s narrative and delves into healing the body’s experience. This mind-body integration is what leads to true, lasting recovery.
- Somatic Healing: Trauma is stored somatically, meaning your body remembers the fear even if your conscious mind does not. By incorporating practices like the Body Scan and mindful movement, TIC helps you gently reconnect with physical sensations. This allows the energy and fear that were stored in the body’s “freeze” response to finally be processed and released in a safe, controlled way. Healing is often experienced not as a cognitive breakthrough, but as a felt sense of calm or release in the body.
- Safety as the Foundation: The pillars of Safety and Trustworthiness are the absolute prerequisites for this deep somatic work. You must trust the container of the therapeutic relationship completely before your nervous system will allow itself to release the frozen survival energy.
A New Relationship with Difficulty
The enduring gift of Trauma-Informed Care is a fundamentally different relationship with suffering.
- From “Why Me?” to “What Now?”: While the pain of the past remains a part of your history, TIC allows you to transition from the paralyzing question of “Why did this happen to me?” to the empowering question of “What do I do now with the strength and wisdom I gained?”
- The Compassion Imperative: You learn that the ultimate act of self-care is self-compassion. When intense emotions inevitably arise, your internalized trauma-informed voice replaces the harsh self-criticism. Instead of thinking, “I’m weak for feeling this way,” you learn to say, “Ah, my nervous system is activated right now because something reminded it of the past. I am safe now, and I can use my skills to soothe myself.”
If you have chosen a trauma-informed path, you have chosen the most respectful and validating journey available. You are not just recovering from trauma; you are establishing a new relationship with yourself—one defined by safety, profound respect, and an unshakable belief in your capacity to heal.
Time to feel better. Find a mental, physical health expert that works for you.
Common FAQs
It’s natural to have questions about an approach as powerful and transformative as Trauma-Informed Care. Understanding TIC helps you advocate for the most compassionate and effective healing environment. Here are answers to common questions about this perspective.
Does Trauma-Informed Care mean I have to talk about my trauma right away?
Absolutely not. TIC emphasizes safety, choice, and control, which means you set the pace for discussing trauma.
- Pacing and Readiness: A trauma-informed professional understands that talking about trauma too soon, or without adequate preparation, can lead to re-traumatization (re-experiencing the event).
- Stabilization First: In TIC, the initial focus is on stabilization and resourcing. This means the therapist will spend weeks, and sometimes months, teaching you concrete skills (like grounding and emotional regulation) so you feel capable of handling intense emotions before you dive into past memories.
- Your Choice is Final: You always have the right to say, “I need to pause,” or “I am not ready to talk about that today,” and a TIC therapist will respect that boundary immediately.
Is TIC a specific type of therapy, like CBT or EMDR?
No, TIC is a philosophy or framework, not a specific technique.
- A Lens, Not a Modality: TIC is best understood as a lens through which any therapy—such as Cognitive Behavioral Therapy (CBT), Dialectical Behavior Therapy (DBT), or even Psychodynamic Therapy—is practiced.
- Safety First: It dictates how the therapy is delivered. For example, a trauma-informed CBT session will prioritize stabilization and choice, ensuring the client is never pushed into challenging thoughts before their nervous system is calm.
- Integration: Many trauma-informed therapists are trained in specific trauma treatment modalities like EMDR, Trauma-Focused CBT (TF-CBT), or Somatic Experiencing (SE), but they always integrate those techniques using the TIC principles of safety and collaboration.
How does TIC address the physical symptoms of anxiety or panic?
TIC recognizes that trauma is stored in the body’s nervous system, not just the mind’s memories.
- The Body Keeps the Score: Your feelings of chronic anxiety, being “on edge,” or easily startled are signs that your nervous system is stuck in survival mode (hyper-arousal or freeze).
- Somatic Focus: TIC uses somatic (body-based) techniques to help you reconnect with your physical self and regulate your nervous system. This often involves:
- Grounding: Exercises that bring you back to the present moment through your senses (feeling your feet on the floor, noticing colors, temperature).
- Body Awareness: Gently noticing where you hold tension (jaw, shoulders, stomach) and learning how to safely release that held energy.
- The goal is to teach your body that the danger is over, which quiets the physical alarm system.
What is the difference between "symptoms" and "survival strategies" in TIC?
This is the core philosophical shift of Trauma-Informed Care.
- Old View (Symptoms): Traditionally, behaviors like intense emotional outbursts, withdrawal, or difficulty trusting were seen as symptoms—signs that something was “wrong” or broken inside you. This often leads to shame and self-blame.
- TIC View (Survival Strategies): TIC reframes these behaviors as intelligent survival strategies—adaptations your brain made to cope with overwhelming situations where safety was compromised.
- Example: Intense outbursts may have been the only way to get attention or protect yourself when you were small and helpless.
- Example: Dissociation (feeling checked out) was a brilliant way for your mind to escape a painful situation your body couldn’t leave.
- The Goal of Reframing: By reframing them as survival strategies, TIC removes the shame and allows you to transition those old, now unhelpful, strategies into new, effective, and adult coping skills.
Why is the therapist so focused on "choice" and "collaboration"?
Choice and collaboration are essential because trauma often involves a profound loss of agency (control over your own life and body).
- Restoring Agency: The therapeutic relationship must explicitly reverse that powerlessness. By giving you control over the session (pacing, topic, veto power), the therapist is symbolically and literally restoring your agency.
- Shared Power: The therapist acts as a collaborator, not a dictator. You are the expert on your internal experience; the therapist is the expert on healing tools. Together, you decide the direction and pace of the work, reinforcing the message: “You are in charge of your life now.”
- This shared power structure is a key factor in building the trustworthiness necessary for trauma survivors.
Can MBSR or CBT be done in a trauma-informed way?
Yes, absolutely. Any evidence-based modality can and should be practiced with a trauma-informed lens.
- Mindfulness (MBSR): A non-informed mindfulness approach might push a client to “sit with the discomfort,” which can be overwhelming for a trauma survivor. A Trauma-Informed Mindfulness approach ensures the client has grounding techniques available, focuses first on finding a safe anchor (like the feeling of the chair) instead of a painful one, and always allows the client to open their eyes or stop the exercise if they feel flooded.
- CBT: A non-informed CBT approach might immediately push a client to challenge a thought like “I am worthless.” A Trauma-Informed CBT approach would first spend time stabilizing the client, validating the feeling (“It makes perfect sense you feel worthless after what happened”), and then gently introducing the thought challenge only after the client has the emotional resources to manage the process safely.
What should I look for to know if a therapist is truly trauma-informed?
Look beyond their credentials and ask practical questions about their approach.
- Ask about Pacing: Do they state clearly that you control the pace of the work?
- Ask about the Body: Do they talk about the nervous system, grounding, or body awareness?
- Ask about Language: Do they use language of collaboration and invitation (“Would you be willing to try…”) rather than directives (“You need to…”)?
- Ask about Boundaries: Are they transparent and clear about confidentiality and fees?
- The Vibe Check: Most importantly, how do you feel in the room? Do you feel respected, heard, and safe? Trust your gut—a trauma-informed space should feel fundamentally safe.
People also ask
Q: What is cognitive behavioural therapy and how does it work?
A: In CBT, the main aim is making changes to solve your problems. In a typical CBT session, you’ll talk about situations you find difficult, and discuss how they make you think, feel and act. You’ll work with your therapist to work out different ways of approaching these situations.
Q:What are the 4 C's of trauma?
A: These 4 Cs are: Calm, Contain, Care, and Cope 2 Trauma and Trauma-Informed Care Page 10 34 (Table 2.3).
Q: What are the 5 stages of trauma healing?
A: The five stages of healing from trauma are the Emergency Stage (immediate survival), the Denial Stage (emotional numbing), the Intrusive Stage (flashbacks and emotional pain), the Transition Stage (active acceptance and starting therapy), and the Long-Term Recovery Stage (consistent management and growth).
Q:What is ABCD in trauma?
A: Airway, Breathing, Circulation, Disability, Exposure. Universal principles for all patients. Apply when critical illness or injury is suspected or evident.
NOTICE TO USERS
MindBodyToday is not intended to be a substitute for professional advice, diagnosis, medical treatment, or therapy. Always seek the advice of your physician or qualified mental health provider with any questions you may have regarding any mental health symptom or medical condition. Never disregard professional psychological or medical advice nor delay in seeking professional advice or treatment because of something you have read on MindBodyToday.
Share this article

Let us know about your needs

Quickly reach the right healthcare Pro

Message health care pros and get the help you need.
Popular Healthcare Professionals Near You
You might also like
What is Face Your Fear and…
, What is Exposure Therapy for Anxiety? Everything you need to know Find a Pro Facing the Fear Monster: A […]
What is Psychodynamic Therapy Explained Guide?
, What is Psychodynamic Therapy Principles? Everything you need to know Find a Pro Digging Deeper: A Simple Guide to […]
What is DBT Therapy Made Simple…
, What is Dialectical Behavior Therapy (DBT) ? Everything you need to know Find a Pro Navigating the Storm: Understanding […]





