What is Healing with Safety and Respect:?
Everything you need to know
Healing with Safety and Respect: Understanding Trauma-Informed Care
If you’re reading this, you’re likely on a journey toward healing, and that is an incredibly brave step. Whether you’re just starting therapy, thinking about it, or are already deep into the process, you might hear the term Trauma-Informed Care (TIC). It might sound like professional jargon, but at its heart, it’s a simple, profound, and essential approach to healing—and it’s something every therapy customer should know about.
This article is for you: the everyday person seeking support. We’ll break down what Trauma-Informed Care means, why it’s vital, and what it should look and feel like in your therapy room, doctor’s office, or any setting where you seek help.
Time to feel better. Find a mental, physical health expert that works for you.
What Is Trauma-Informed Care, Really?
To understand Trauma-Informed Care, we must first understand how trauma impacts a person. Trauma, broadly defined, is an experience or series of experiences that overwhelm a person’s capacity to cope. It’s an event that leaves the person feeling helpless, terrified, or profoundly unsafe. Importantly, it’s not the event itself, but the person’s response to the event that determines if it is traumatic.
Imagine you have a complex injury, like a broken bone that didn’t heal quite right. Trauma-Informed Care isn’t just about fixing the current pain (like anxiety or depression); it’s about recognizing that the underlying injury (trauma) affects everything—how you move, how you react to touch, and how much you trust the doctor.
In simple terms, Trauma-Informed Care is an approach where every person providing a service operates with the understanding that the person they are helping may have a history of trauma. This understanding applies to every level of service, from the receptionist who schedules your appointment to the therapist in the room.
It’s not about forcing you to talk about your trauma. It’s about changing the fundamental question from:
“What is wrong with you?” (Focusing on symptoms and diagnosis)
to the healing question:
“What happened to you?” (Focusing on the person’s history and experience)
This shift in perspective changes everything about how support is delivered. It moves away from judgment and toward compassion, safety, and empowerment. When a provider asks “What happened to you?” they see symptoms like avoidance, intense anger, or difficulty sleeping not as flaws, but as understandable survival strategies developed to cope with overwhelming events.
Why Is Trauma-Informed Care So Important for You?
You might think, “I’m here for anxiety, not trauma.” But research shows that trauma is incredibly common. The groundbreaking Adverse Childhood Experiences (ACEs) study revealed that a majority of adults have experienced at least one adverse childhood event, and many have experienced four or more.
This means a majority of people seeking mental health treatment have experienced some form of trauma—even if they don’t consciously label it as such. Trauma isn’t just major events like war or abuse; it can be emotional neglect, bullying, medical procedures, poverty, or a consistent feeling of being unsafe.
The Body Keeps the Score: Trauma’s Physical Impact
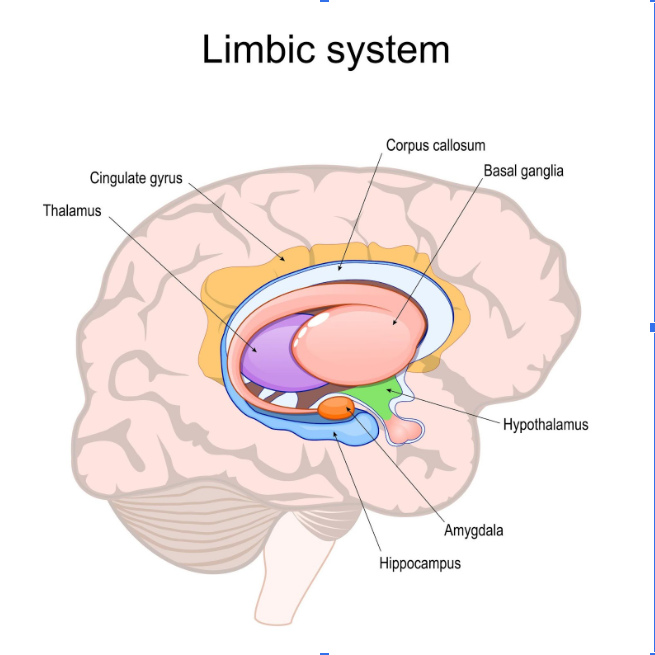
When you experience trauma, your brain and body change the way they handle stress and danger. The part of your brain responsible for survival, the amygdala, becomes hyperactive. Your nervous system learns to be on high alert all the time, constantly scanning the environment for threats. This state is known as hyperarousal.
This persistent state of defense and reactivity can show up in your life as:
- Intense anxiety or panic (feeling constantly threatened even when safe).
- Difficulty trusting (because you learned people or situations aren’t safe).
- Emotional numbness or detachment (a way your system uses to cope with overwhelming feelings).
- Physical symptoms (headaches, stomach issues, chronic pain, or chronic fatigue).
- Hypersensitivity to noise, touch, or certain tones of voice (which the body interprets as signs of danger).
If a therapist or caregiver doesn’t understand these effects, they could accidentally do something that re-traumatizes you—meaning they trigger a painful memory, a state of hyperarousal, or put you in a position that feels scary and unsafe (like forcing eye contact or rushing you to share details), setting back your healing. TIC is designed specifically to prevent this by prioritizing stability and choice.
Connect Free. Improve your mental and physical health with a professional near you

The Six Core Principles: What to Look For
Trauma-Informed Care isn’t just a general nice idea; it’s based on a specific set of principles developed by the Substance Abuse and Mental Health Services Administration (SAMHSA). These principles are the practical ways a professional can create a healing environment. As a client, you have the right to look for these qualities in your care:
-
Safety (Physical and Emotional)
This is the non-negotiable foundation. You need to feel safe in the physical setting and with the person helping you. If your nervous system perceives danger, healing cannot happen.
- In Practice: The physical space should feel calm, private, and arranged so you don’t feel trapped (e.g., you can easily see the door, not seated with your back to it). The professional speaks calmly and maintains predictable, professional boundaries. Most importantly, they assure you that you have control and can stop talking about anything at any time, protecting your emotional safety.
-
Trustworthiness and Transparency
Trauma often involves betrayal, secrets, or unpredictable behavior from others. Therefore, a healing environment must be clear, honest, and reliable to rebuild trust.
- In Practice: Your therapist explains the rules of confidentiality clearly and upfront, including the few exceptions where they might have to break it (duty to warn, etc.). They tell you the purpose of a particular exercise or homework assignment before you do it. They are transparent about their fees, scheduling, and what the overall treatment plan will look like. No surprises are the rule of thumb.
-
Peer Support
The experience of trauma can be intensely isolating. Peer support involves sharing and learning from others who have similar experiences, which can reduce isolation and offer tangible hope that recovery is possible.
- In Practice: This could mean the care provider encourages or offers referrals to support groups, or employs staff who have lived experience with trauma and recovery (peer specialists) who can offer unique empathy and perspective.
-
Collaboration and Mutuality
This is a key shift from the old medical model where the doctor or therapist was the sole “expert” and the client just followed orders. In TIC, healing is a partnership. You are the expert on your own experience and needs.
- In Practice: Your goals are central. The therapist doesn’t tell you what to work on; you work together to set the agenda for each session. You are actively involved in designing your treatment plan and setting the pace. The professional checks in regularly: “How did that exercise feel for you?” or “Is this pace working for you?”
-
Empowerment, Voice, and Choice
Trauma often involves a profound loss of control, where a person’s voice and choices are taken away. Rebuilding that sense of agency (the ability to act and make choices) is crucial for healing.
- In Practice: The therapist always gives you choices: “Would you like to start with this topic, or would you prefer we review your week first?” They respect your pace. If you say, “I’m not ready to talk about that yet,” they accept it without pressure or judgment. They focus on your strengths and resilience, highlighting how you have already survived difficult events, rather than just focusing on your symptoms or deficits.
-
Cultural, Historical, and Gender Issues
Acknowledging that culture, historical trauma (like systemic oppression, racism, or generational hardship), gender, sexual orientation, and race deeply impact how trauma is experienced and how healing occurs. The environment must be sensitive and responsive to these diverse backgrounds.
- In Practice: The professional is aware of and sensitive to your cultural background and how it influences your worldview and coping mechanisms. They don’t generalize or dismiss experiences related to discrimination or historical injustice, recognizing that systemic harm is a form of trauma. They actively strive to provide care that is non-discriminatory and relevant to your unique identity.
What Trauma-Informed Care Is NOT
Understanding what TIC is not can be just as important as knowing what it is:
- It is NOT Trauma Therapy: TIC is a way of delivering care, a lens through which all interactions should occur. It is not a specific treatment for trauma like EMDR, Somatic Experiencing, or Cognitive Processing Therapy (CPT). A TIC therapist will use specialized trauma treatments when appropriate, but the TIC principles are the foundation for all their work.
- It is NOT Avoiding Difficult Topics: Being trauma-informed doesn’t mean you avoid talking about hard things forever. It means that when you do approach difficult memories, the professional ensures you have the safety, stabilization, and grounding skills needed first, and that you are always in control of the pace.
- It is NOT an Excuse: Being trauma-informed doesn’t mean excusing destructive behavior; it means understanding the behavior (like substance use or emotional outbursts) as a survival strategy that is no longer effective. It allows the therapist to gently hold you accountable for change while maintaining compassion for the reasons behind the behavior.
Using Your Power: Taking Agency in the Healing Process
The most empowering aspect of Trauma-Informed Care is that it gives you, the client, back your agency. You are not a passive recipient of treatment; you are an active collaborator.
Here are a few ways you can practice your own TIC principles in your therapy:
- Practice Your Voice: If you don’t like a therapeutic exercise, say “I’d like to try something different.” If the room is too cold, ask for a blanket. If a topic is too much, say “Stop.” Your therapist should honor this immediately.
- Insist on Transparency: If you don’t understand the purpose of a homework assignment, ask, “What is the goal of this exercise?” You have the right to understand why you are doing something and how it relates to your goals.
- Prioritize Safety: If you leave a session feeling activated, highly distressed, or emotionally dysregulated, bring that up the next time. A trauma-informed therapist will see this as valuable feedback and adjust their approach, perhaps by focusing more on grounding and stabilization skills before moving to deeper emotional work.
Healing from trauma is an incredible act of courage. By understanding the principles of Trauma-Informed Care, you are not just learning about therapy—you are learning how to advocate for yourself, choose safe spaces, and participate actively in your own well-being. You deserve a care setting where you are seen not as a problem to be fixed, but as a resilient, whole person whose past experiences deserve respect and understanding.

Free consultations. Connect free with local health professionals near you.
Conclusion
Reclaiming Your Agency Through Trauma-Informed Care
You have journeyed through the core principles of Trauma-Informed Care (TIC), moving from simple definition to understanding its profound, body-level impact. This conclusion is not an ending, but a synthesis of your newfound knowledge—a guide to integrating these principles as you move forward in your healing process. Ultimately, embracing TIC is about reclaiming your personal agency and insisting on safety, respect, and choice in every care setting you encounter.
The Paradigm Shift: From Pathologizing to Understanding
The most enduring takeaway from understanding TIC is the fundamental shift from viewing yourself as “flawed” to viewing yourself as “injured.” This paradigm shift is liberating:
|
Old, Pathologizing View (Pre-TIC) |
New, Trauma-Informed View (TIC) |
|---|---|
|
“What is wrong with me?” |
“What happened to me?” |
|
Symptoms (e.g., panic attacks, anger) are seen as failures of control. |
Symptoms are seen as natural, though perhaps outdated, survival strategies. |
|
The client is expected to adapt to the service. |
The service must adapt to the client’s trauma history and need for safety. |
|
The professional is the sole expert. |
The client and professional are collaborative partners in healing. |
When you understand that your intense anxiety is your nervous system shouting a loud warning learned during a terrifying past experience
term mental wellness.

, you can treat that anxiety with curiosity and compassion, not self-loathing. This perspective is the necessary fuel for any successful trauma recovery.
Why Safety and Choice Are Non-Negotiable
The six core principles of TIC—Safety, Trustworthiness, Peer Support, Collaboration, Empowerment, and Cultural Sensitivity—all work toward one vital goal: counteracting the effects of trauma.1
Trauma, by definition, involves being overwhelmed, having your safety violated, and losing control over your own body and circumstances. Therefore, the healing environment must meticulously provide the opposite experience.
- Safety (The Sanctuary): Your body and mind need a place where the hyperactive alarm system (the amygdala) can finally stand down. A physically and emotionally predictable environment allows the nervous system to relax and shifts your state from fight/flight/freeze to “rest and digest.” Without this foundation, any deep emotional work becomes re-traumatizing.
- Empowerment and Choice (The Steering Wheel): If your past involved powerlessness, every single opportunity to exert choice in the present is a corrective emotional experience.2 A trauma-informed therapist knows that offering a choice—“Would you like to sit closer to the door?”, “Can we pause here?”, or “You don’t have to share anything you aren’t ready to share”—is not just being polite; it is an active therapeutic intervention that rebuilds your sense of self-agency.3Your “no” must be honored immediately and without question.
Integrating TIC: You Are the Advocate
Knowing these principles is not just about judging your therapist; it’s about becoming your own fiercest advocate. In the healing process, you are your own primary care provider, and you deserve a high-quality service.
If you are already in therapy, use your knowledge of TIC to assess the health of the therapeutic relationship:
- Check for Transparency: Does your therapist explain the why behind their methods? Do they clearly communicate boundaries and scheduling? A lack of transparency can feel unsettling and erode trust—bring it up if you notice it.
- Evaluate Collaboration: Are you a passenger or a co-pilot? If you feel the therapist is rushing you, pushing an agenda that doesn’t align with your current goals, or minimizing your input, your collaboration is lacking. Remember, you set the pace.
- Monitor Your Body: Your body is the expert on your trauma. If you leave a session feeling intensely drained, highly activated, dizzy, or numb, your body is telling you that the work may have moved too quickly or lacked sufficient grounding. Use your next session to discuss that physical experience, not just the content. A trauma-informed therapist will immediately prioritize skills to help you regulate that feeling.4
The Broader Scope of Trauma
Finally, remember that Trauma-Informed Care extends far beyond the mental health office.5 As a client, you might interact with professionals who are trauma-informed and those who are not.
- Trauma-Informed Doctor: Will explain a medical procedure step-by-step, warn you before touching you, and give you control over position (Choice).6
- Non-Trauma-Informed Doctor: Rushes you, performs a procedure without adequate warning, or dismisses your pain (Loss of control/safety).
By carrying the TIC lens with you, you become empowered to seek out and demand safe, respectful care from every person and institution you interact with. This is not about being difficult; it is about establishing the non-negotiable standards required for your body and mind to heal.
Healing is a testament to your resilience. It’s an act of courage to move through the world and pursue wellness, especially when that world has previously failed to protect you. By insisting on Trauma-Informed Care, you are ensuring that your healing journey is one of safety, dignity, and self-reclamation. You are worthy of this level of care.
Time to feel better. Find a mental, physical health expert that works for you.
Common FAQs
Understanding Trauma-Informed Care is a vital step in advocating for your healing. Here are clear, simple answers to the most common questions people ask about this approach.
What is the single most important idea in Trauma-Informed Care (TIC)?
The most important idea is the shift in perspective from asking “What is wrong with you?” to asking “What happened to you?” TIC recognizes that symptoms like anxiety, anger, or avoidance are often understandable survival strategies developed to cope with past overwhelming or unsafe experiences (trauma). This changes the relationship from one of judgment to one of compassion and collaboration.
Does a therapist practicing TIC have to be a trauma specialist?
No. TIC is a universal approach or a philosophy of care that should be practiced by all staff in any organization (therapists, doctors, receptionists, etc.). A TIC-informed therapist will always prioritize safety, choice, and stability. While they may not use specialized trauma treatments (like EMDR or CPT), they will ensure the way they deliver therapy prevents re-traumatization.
If I haven't been diagnosed with PTSD, do I still need Trauma-Informed Care?
Yes, absolutely. Trauma is a widespread issue that affects the body and mind in many ways, even if you don’t meet the criteria for Post-Traumatic Stress Disorder (PTSD). Trauma includes things like childhood neglect, chronic stress, medical trauma, or ongoing discrimination. If you struggle with trust, intense anxiety, emotional regulation, or feeling safe in your body, a TIC approach will be beneficial because it focuses on these core issues.
How does trauma physically affect my body, and why does my therapist need to know this?
Trauma keeps your nervous system in a state of high alert, primarily involving the amygdala (the brain’s danger detector). This state of hyperarousal

means your body reacts to current, minor stress as if it were a major, life-threatening danger. A TIC therapist understands that your body’s reaction (like rapid heart rate, freezing, or intense flushing) is not a choice, but a biological survival response. They will teach you grounding skills to help your nervous system calm down before diving into emotional work.
Common FAQs
Principles and Practice
What are the three most important things I should look for in a therapy setting to ensure it is trauma-informed?
Look for evidence of these core principles:
- Safety: Both physical comfort (a private, calm room) and emotional safety (the therapist is predictable and maintains clear boundaries).
- Choice: The therapist constantly offers you control over the session. They ask: “Would you like to stop?” or “Do you want to approach this now?”
- Collaboration: You feel like an active partner. The therapist doesn’t tell you what to do but works with you to set goals and decide the pace.
Why is choice so important in trauma recovery?
Trauma often involves an experience where the victim was powerless and had their choices taken away. By consistently offering choices—even small ones like “Where would you like to sit?” or “Do you want to use the tissue box?”—the therapist helps you rebuild your sense of agency and control. This corrective experience is crucial for healing the deep wounds of powerlessness.
7. What if I want to talk about my trauma details right away? Will a TIC therapist allow this?
A true TIC approach emphasizes stabilization before processing. A trauma-informed therapist will gently slow down the pace if you are rushing to share painful details. They will first ensure you have reliable grounding and containment skills (Distress Tolerance) to manage the intense emotions that often surface during trauma processing. Sharing too much, too fast, without these skills can be re-traumatizing. The therapist is protecting your safety.
How can I, as the client, practice the principles of TIC in my own healing?
You can practice TIC by becoming your own advocate and taking agency:
- Use Your Voice: Practice saying “I need a break” or “I’m not ready to talk about that.”
- Insist on Transparency: Ask your therapist, “What is the goal of this exercise and how does it help me reach my goals?”
- Listen to Your Body: Pay attention to physical signs of stress (tightness, holding your breath, numbness) and communicate those signals to your therapist.
Common FAQs
Logistics and Commitment
Can I ask a potential therapist if they are "trauma-informed"? What should I listen for in their answer?
Yes, you absolutely should ask! A good answer will be simple and practical. Listen for them to mention concepts like:
- “I always prioritize your safety and control over the session.”
- “We will work collaboratively to set the pace and goals.”
- “I check in with you regularly to see how your body is feeling.”
- “We will spend time on grounding skills before tackling difficult topics.”
A poor answer would be one that is vague, overly academic, or focuses only on a specific trauma treatment without mentioning the core principles of safety and choice.
Does TIC mean my therapist will let me get away with destructive behavior because "it's the trauma?"
No. TIC recognizes that destructive behaviors (like lashing out, using substances, or self-harm) are often desperate attempts to cope with overwhelming emotional pain. The professional’s job is not to excuse the behavior, but to understand its roots, validate the pain, and then gently and collaboratively hold you accountable for learning new, effective coping skills. The principle of collaboration means working together to replace those old survival strategies with new, healthier choices.
People also ask
Q: What are the 5 concepts of trauma-informed care?
A: The five guiding trauma-informed values and principles proposed by Drs. Maxine Harris and Roger Fallot are safety (physical and emotional), trustworthiness, choice, collaboration and empowerment.
Q:What are the 4 elements of trauma-informed care?
A: Trauma-informed care is revolutionizing our understanding and approach to trauma, emphasizing a compassionate, empathic view that enriches mental health services. At its core are the foundational 4 Rs: Realization, Recognize, Respond, and Resist Re-traumatization.
Q: What are the 6 key principles of trauma-informed care?
A: The principlesa are safety, trustworthiness and transparency, peer support, collaboration and mutuality, empowerment and choice, and humility. These principles can be used in clinical and mental health care settings, workplaces, educational institutions and other organizations.
Q:What are the 7 elements of a trauma-informed club?
A: This award recognizes programs that integrate and are guided by the seven elements of a trauma-informed Club: 1) Awareness, 2) Safety, 3) Trust, 4) Equity, 5) Empowerment, Voice & Choice, 6) Mutual Collaboration, and 7) Connection & Growth.
NOTICE TO USERS
MindBodyToday is not intended to be a substitute for professional advice, diagnosis, medical treatment, or therapy. Always seek the advice of your physician or qualified mental health provider with any questions you may have regarding any mental health symptom or medical condition. Never disregard professional psychological or medical advice nor delay in seeking professional advice or treatment because of something you have read on MindBodyToday.
Share this article

Let us know about your needs

Quickly reach the right healthcare Pro

Message health care pros and get the help you need.
Popular Healthcare Professionals Near You
You might also like
What is Psychodynamic Therapy Principles?
, What is Psychodynamic Therapy Principles?Everything you need to know Find a Pro Digging Deeper: A Simple Guide to Psychodynamic […]
What is Dialectical Behavior Therapy (DBT)?
, What is Dialectical Behavior Therapy (DBT) ? Everything you need to know Find a Pro Navigating the Storm: Understanding […]
What is Cognitive Behavioral Therapy (CBT)?
, What is Cognitive Behavioral Therapy (CBT) ? Everything you need to know Find a Pro Your Thoughts Are Not […]





