Healing Starts Here: Understanding Trauma-Informed Care
If you’re considering therapy, or already on your healing journey, you’ve likely come across the term “trauma.” Trauma isn’t just about big, dramatic events like natural disasters or combat; it’s any deeply distressing or disturbing experience that overwhelms your ability to cope, leaving lasting emotional, psychological, and even physical impacts. In fact, a vast majority of people—around 70%—have experienced some form of trauma in their lives, which means that the therapy room is almost certainly filled with survivors.
Because trauma is so widespread and profoundly affects how the brain and body function, the mental health field has shifted toward a new, essential standard of care called Trauma-Informed Care (TIC).
Trauma-Informed Care is not a specific type of therapy (like CBT or EMDR); rather, it’s a fundamental way of seeing the world and interacting with people. It’s a complete cultural shift in how an organization or a therapist operates. It changes the focus from “What is wrong with you?” to “What happened to you?” This shift acknowledges that most behaviors that look like symptoms are actually brilliant, albeit sometimes messy, survival strategies.
Time to feel better. Find a mental, physical health expert that works for you.
This shift is crucial because if you’ve been through painful or frightening experiences, your priority is—and always should be—safety and control. Trauma-Informed Care recognizes that your past experiences fundamentally shape your present needs, reactions, and behaviors in the therapy room and in life. It assumes that anyone walking through the door may have a trauma history and acts accordingly to prevent re-traumatization.
This article is your warm, supportive, and practical guide to understanding what Trauma-Informed Care is, why it matters, and how you can recognize if your therapist and their practice are truly trauma-informed.
Part 1: Why Trauma Changes Everything
To understand Trauma-Informed Care, we first need a simple understanding of how trauma affects the brain and body. Trauma changes the way your internal alarm system operates.
Trauma and the Survival Brain
When you experience trauma, your brain’s emotional center—the amygdala—goes into overdrive, perceiving an immediate threat. Your rational, thinking brain (the prefrontal cortex) steps back, and your survival brain takes complete control. This triggers the famous “fight, flight, freeze, or fawn” response.
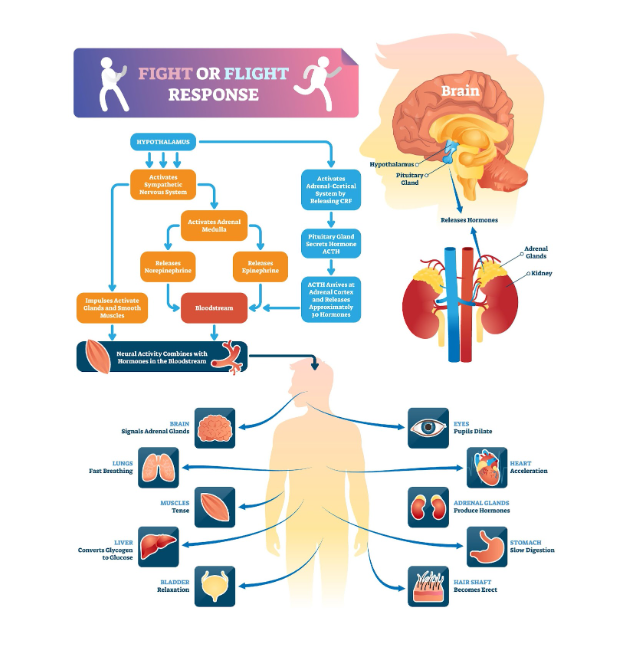
- The Freeze/Fawn Response: Often in situations where escape or fighting back is impossible (like childhood abuse, neglect, or chronic emotional invalidation), the brain shifts into a “freeze” state (shutting down) or a “fawn” state (trying to please the aggressor to ensure survival). This is a brilliant survival mechanism, but it leaves the body holding onto the stress and fear long after the threat is gone.
- Hypervigilance: Trauma changes your internal baseline. Your nervous system stays “on high alert” (hypervigilance) because your brain is tirelessly trying to protect you from the possibility of the past happening again. This state can manifest as chronic anxiety, difficulty relaxing, explosive anger (fight response), avoidance (flight response), or feeling disconnected from your body (freeze response).
Trauma and Trust
For many survivors, especially those with complex trauma (repeated trauma over a long period, often in childhood and involving betrayal), the world and the people in it feel fundamentally unsafe. Authority figures, close relationships, and even safe, quiet environments can feel dangerous because the brain equates the present moment with past pain.
This is why traditional therapy—which often involves vulnerability, authority, and deep disclosure—can sometimes feel scary or even accidentally re-traumatizing if it isn’t handled with extreme care. Trauma-Informed Care is specifically designed to counteract these biological and psychological effects by prioritizing safety and control above all else.
Part 2: The Core Principles of Trauma-Informed Care
Trauma-Informed Care (TIC) operationalizes the understanding of trauma through a set of guiding principles. For a client, these principles translate directly into the high-quality, ethical care you deserve.
- Safety (Physical and Emotional)
This is the non-negotiable foundation. If your nervous system perceives a threat, healing stops.
- Physical Safety: This addresses the environment. Is the therapy office private, clean, and comfortable? Is the seating arranged so you can sit closest to the door if that makes you feel safer? Are there clear, accessible pathways?
- Emotional Safety: This is paramount. It means the therapist ensures you never feel shamed, judged, or pressured to disclose more than you are ready to. They validate your feelings and reactions without labeling them as disproportionate or pathological. They understand that a reaction that seems extreme is simply a normal response to an abnormal, overwhelming past event.
- Trustworthiness and Transparency
Trauma often involves breaches of trust and betrayal, so the healing environment must be predictable, honest, and reliable.
- Clear Boundaries: The therapist is impeccably clear about appointment times, fees, cancellation policies, and, most importantly, the limits of confidentiality. There are no “gotchas” or sudden rule changes.
- Transparency: The therapist explains why they are using a particular technique. For example, instead of suddenly asking you to close your eyes, a trauma-informed therapist might say, “We are going to try this breathing exercise because it helps regulate the vagus nerve, which is often stuck in overdrive after trauma. I want you to know you are always free to keep your eyes open or stop if it feels uncomfortable.” This approach respects your right to know and anticipate what will happen.
Connect Free. Improve your mental and physical health with a professional near you

- Collaboration and Mutuality (Putting You in Control)
Since trauma involves being powerless and having choices taken away, healing must involve regaining power and control. Trauma-Informed Care works with you, seeing you as the ultimate expert on your life.
- Shared Decision-Making: The therapist sees you as a partner. You decide which issues to tackle, when to slow down, and which specific techniques (e.g., grounding, EMDR, Somatic work) to try. A trauma-informed therapist will never demand you recount a traumatic memory before you have developed solid coping and grounding skills.
- Pacing and Choice: You always have the absolute right to say “no,” to take a break, or to shift the topic. Pacing is key: the therapist honors your readiness, recognizing that forcing disclosure can re-trigger and re-traumatize.
- Empowerment and Voice
The goal is to reinforce your inherent strengths and validate your ability to make your own decisions and solve your own problems.
- Focus on Strengths: Trauma-Informed Care actively searches for and highlights your resilience, survival skills, and current successes. The narrative shifts from “I am damaged” to “I am a survivor who developed incredible, protective strategies to cope, and now we can update those strategies.”
- Advocacy: The therapist recognizes that your struggles may be linked not just to personal history but to systemic issues (poverty, racism, discrimination, violence) and will advocate for resources or acknowledge the external impact of these forces on your mental health.
Part 3: How to Spot a Trauma-Informed Therapist (Practical Signs)
A truly trauma-informed practice will show specific, observable behaviors from the very first interaction. You don’t need a certificate on the wall; you need evidence in the actions.
During the Intake and Assessment
- The Question Shift: They don’t just focus on the list of your current symptoms. They ask questions that seek to understand the history and context of your distress (the “What happened?”). They will inquire about your childhood safety, experiences with neglect, past losses, or experiences of discrimination, always asking gently and allowing you to decline answering.
- Explicit Consent: They are meticulous about Informed Consent. They clearly explain the limits of confidentiality, their fees, and their clinical approach before you start sharing sensitive details, ensuring there is a predictable framework.
- Prioritizing Stabilization: If you mention a traumatic event, their first question is often: “Are you grounded right now? Are you ready to talk about that today, or should we focus on building coping skills first?” They prioritize stabilization over immediate disclosure.
In the Session Itself
- Modeling Calm: The therapist maintains a calm, regulated presence. They don’t react to your emotional spikes with their own fear or sudden shifts in tone. They are a stable anchor in the room, helping your nervous system co-regulate with theirs.
- Language of Choice: They constantly use language that reinforces your control: “Where would you like to sit?” “We can take a five-minute break now if you need it.” “Tell me what we should work on today. You decide the pace.”
- Body Awareness (Somatic Focus): They pay attention to your body language. If you tense up, shift, or freeze, they might gently ask, “I notice your hands are gripping the chair. What is your body telling you right now? Can we use a grounding skill to bring your awareness back to the room?” This acknowledges that the body holds the memory and invites you to listen to it safely.
- Grounding Check: They ensure you have reliable grounding techniques (skills to connect you back to the safety of the present moment) before discussing triggering material, and they always check to ensure you are grounded and present before ending the session.
The Office Environment
- A Welcoming Space: The physical office space should feel calm, not chaotic. Lighting should be adjustable, seating should be comfortable, and there should be a clear emphasis on privacy.
- Accessibility of Comfort: Items like water, tissues, or even a soft blanket should be readily available without you having to ask, minimizing any potential feelings of neediness or awkwardness.
- Privacy: The therapist ensures conversations cannot be overheard in the waiting area or from neighboring offices.
Part 4: Trauma-Informed Care as a Ladder to Healing
Trauma-Informed Care is not a replacement for specialized trauma treatment (like EMDR, Somatic Experiencing, or TF-CBT), but it is the essential prerequisite for it.
Stabilization is Job One
Think of healing trauma as climbing a ladder. If the ground is shaking, you can’t get on the ladder to climb. Trauma-Informed Care provides the stable ground.
The first phase of all ethical trauma treatment is Stabilization. This phase, which is entirely guided by TIC principles, focuses on:
- Establishing Safety (ending any ongoing unsafe situations).
- Building the Toolkit (mastering grounding, breathing, and emotional regulation skills).
- Developing a Stable, Trusting, and Transparent Relationship with the therapist.
Without these trauma-informed stabilization steps, attempts to process the trauma memory can be overwhelming, overwhelming the client’s already overloaded nervous system, and potentially leading to re-traumatization.
The Long-Term Impact
For you, the client, choosing a Trauma-Informed approach leads to long-term gains:
- Reduced Shame: By shifting the focus from “what’s wrong” to “what happened,” the shame and self-blame that often accompany trauma begin to dissipate, allowing for self-compassion.
- Increased Self-Trust: By having your choices respected and your reactions validated, you learn to trust your own body and instincts again—the very systems that were corrupted by the trauma.
- Effective Treatment: When the foundation is safe, specific trauma therapies can be introduced effectively, leading to deep, lasting reprocessing and relief, integrating the past into a coherent narrative.
Your past experiences are not a reflection of your character; they are a testament to your ability to survive. By choosing a trauma-informed approach, you are choosing a path where your survival story is honored, and your future is defined by safety, collaboration, and empowerment.

Free consultations. Connect free with local health professionals near you.
Conclusion
The Final Act: A Detailed Look at the Conclusion of Trauma-Informed Care
The conclusion of any therapeutic journey is a significant milestone, but in the context of Trauma-Informed Care (TIC), termination carries unique ethical and clinical weight. Since the core of trauma involves issues of safety, control, and trust, the final phase of therapy must be managed meticulously to ensure the client is empowered and that the ending itself does not feel like a repetition of past abandonment or powerlessness.
Trauma-Informed Care is a framework, not a time-limited treatment. Therefore, the conclusion of the relationship is based on the client’s successful transition from the stabilization phase to either a full trauma processing phase or a successful return to independent living, all while maintaining the principles of safety and collaboration.
This article details the specific, trauma-informed criteria that signal readiness for termination, the crucial steps the therapist takes to consolidate the client’s gains in safety and self-efficacy, and the essential mindset required for maintaining resilience post-therapy.
Markers of Ethical Readiness: Defining Safety and Stability
The decision to conclude a relationship rooted in Trauma-Informed Care is based on the professional assessment that the client has achieved sustained, internalized safety and control, reducing the chronic hypervigilance that trauma creates.
- Internalized Safety and Emotional Regulation
The client must demonstrate that their internal alarm system is effectively managed and no longer dictating their daily life.
- Effective Grounding: The client has mastered several grounding and calming techniques and uses them automatically whenever they feel triggered or distressed. They are consistently able to bring themselves back to the present moment without external help.
- Reduced Hypervigilance: The client reports a significant, sustained reduction in chronic anxiety, sleep disturbances, and hyper-arousal. Their baseline state is one of calm, not alert.
- Tolerable Emotional Range: The client can experience difficult emotions (sadness, anger, fear) without dissociating, freezing, or resorting to destructive coping mechanisms. They can “ride the wave” of emotion without being swept away, demonstrating mastery of the Stabilization phase.
- Restored Control and Collaboration
The client has reclaimed agency and control over their lives and their therapeutic process.
- Client-Directed Narrative: The client can discuss their trauma history (or choose not to) without feeling pressured, overwhelmed, or re-traumatized. They dictate the pace and content of sessions, knowing their therapist will honor their boundaries (demonstrating successful Collaboration).
- Restored Self-Trust: The client trusts their own instincts and body signals again. They rely less on the therapist for validation and trust their own judgment in making life decisions, having successfully challenged the trauma-driven narrative of powerlessness.
- Healthy Boundaries in Life: The client is successfully implementing and maintaining clear, healthy boundaries in their personal and professional relationships, reducing the risk of further relational trauma.
- Transition Readiness
The focus has shifted from managing the past to actively living in the present and planning for the future.
- Value-Driven Living: The client is consistently engaging in activities that align with their personal values, indicating that they are motivated by life goals rather than avoiding trauma triggers.
- Positive Future Orientation: The client expresses a sense of hope, purpose, and a belief that the future will be safe and meaningful, a stark contrast to the despair and foreshortened future often seen in survivors.
Final Interventions: Consolidating Safety and Empowerment
The final sessions are not simply a review, but a highly specific phase designed to anchor the client’s gains in safety and autonomy, directly counteracting the long-term impact of trauma.
- The Ethical Processing of Termination
Since trauma often involves abrupt abandonment or rupture, the ethical conclusion must be a planned, collaborative, and fully processed ending.
- The Dialogue of Loss: The therapist proactively opens the discussion about the conclusion, allowing the client ample time (several sessions) to express any feelings of loss, fear, or sadness without judgment. The therapist must remain regulated and present during this discussion, modeling a healthy, time-limited, and reparative ending.
- Internalizing the Safe Base: The final goal is to help the client internalize the safety and compassion provided by the therapist. The client should leave with the feeling that the safety they experienced in the relationship can now be accessed within themselves.
- Future-Pacing Safety and Triggers
Drawing on the principles of predictability and competence, the final phase ensures the client is prepared for inevitable future stressors.
- Anticipating Rupture: The therapist and client work together to predict potential future events that might feel like a breach of safety or trust (e.g., a friend suddenly ghosting them, a medical procedure). For each scenario, they identify the specific grounding skill, boundary setting skill, and cognitive reframing the client will use. This ensures the client has a prepared response, thereby retaining control.
- The “If-Then” Plan: The plan is framed as: “If I notice my body starting to freeze (a trauma response), then I will immediately use the 5-4-3-2-1 technique (a grounding skill) and remind myself, ‘That was then, this is now, and I am safe.’ (a cognitive reframing).” This creates a powerful, automatic counter-response to trauma triggers.
- Review of the Trauma Narrative (The “Blueprint”)
The final sessions involve creating a mental and/or physical blueprint of the healing journey, framed entirely through the lens of strength.
- Highlighting Resilience: The therapist reviews the client’s journey, explicitly pointing out the moments of immense courage, resilience, and successful self-advocacy. The focus is on “You did this, you chose safety, you built these skills.”
- The Shift from Victim to Survivor/Thriver: This final review solidifies the client’s identity as a survivor who overcame profound adversity and is now capable of facing the future not despite their past, but empowered by the resilience their survival required. The narrative is not about the trauma itself, but about the client’s strength in navigating it.
Maintaining Freedom: Living an Empowered Life Post-TIC
The conclusion of therapy based on Trauma-Informed Care means the client has transitioned to being their own primary agent of safety, control, and healing.
- Commitment to Daily Self-Care as Safety
For trauma survivors, self-care is not a luxury; it is a safety protocol. The client commits to maintaining the skills that keep their nervous system regulated.
- Grounding Check-ins: Routine daily mindfulness or grounding checks are used to prevent the hypervigilance response from creeping back into the baseline.
- Boundary Maintenance: Continuous practice of clear communication and boundary setting is essential to prevent future relational wounds. The client learns that protecting their own safety is a lifelong, ethical responsibility to themselves.
- The Power of Consultation
The client should establish healthy, reliable consultation resources outside of the professional relationship (trusted friends, partners, mentors) who understand the importance of validation and safety, ensuring the client has a network that reinforces the principles learned in therapy.
The conclusion of therapy within a Trauma-Informed framework is the ultimate act of empowerment. It affirms that the client is not only healed from the wound but is now equipped with the integrated safety protocols necessary to navigate a complex world with confidence, self-trust, and autonomy.
Time to feel better. Find a mental, physical health expert that works for you.
Common FAQs
If you’ve completed or are nearing the end of therapy that prioritized Trauma-Informed Care (TIC), you likely have questions about what success looks like, how to handle the emotional intensity of termination, and how to maintain the safety and control you’ve worked so hard to establish.
How do we know therapy rooted in Trauma-Informed Care is finished?
Since TIC is a framework, the conclusion is based on achieving safety and stability, which are the prerequisites for deeper healing. The therapy is generally ready to conclude when:
- Safety is Internalized: You have mastered grounding and calming techniques and use them automatically, demonstrating a sustained reduction in hypervigilance and anxiety.
- Control is Restored: You consistently assert your boundaries, make autonomous choices, and feel like you are driving your life, not just reacting to triggers.
- Stabilization is Complete: If the goal was full trauma processing (like EMDR), that phase is finished, and you have integrated the experience without feeling overwhelmed or unsafe.
- The Narrative Shifts: You consistently view yourself as a survivor/thriver, not primarily as a victim.
Is it normal to feel anxious or abandoned when the therapist suggests ending?
Yes, this is an expected and important part of the ethical termination process, especially in TIC.
- Trauma Repetition: Since trauma often involves experiences of betrayal, abandonment, or loss of control, the ending of a safe relationship can easily trigger those old feelings.
- Ethical Processing: A trauma-informed therapist will dedicate final sessions to processing this termination thoroughly. They model a healthy, predictable, and reparative ending, ensuring the final memory of the relationship is one of safety and mutual respect, not abrupt loss.
How does the therapist ensure the ending doesn't feel re-traumatizing?
The therapist uses the core principles of TIC right up to the final minute:
- Collaboration and Choice: You are given ample notice, and the timing of the end is collaborative. You are never surprised or dropped without warning.
- Transparency: The therapist is transparent about the process, explaining why the relationship needs to end (i.e., you achieved your goals and are ready for autonomy).
- Future-Pacing Safety: The therapist helps you create an “If-Then” plan for future crises, explicitly teaching you how to use your internalized skills to maintain safety, preventing the feeling of being left powerless.
What is the most important thing I take away from this kind of care?
You take away Internalized Safety and Self-Trust.
- Internalized Safety: You learn that the ultimate source of safety is not the therapist, but your own nervous system and your ability to regulate it using your mastered grounding skills.
- Self-Trust: By having the therapist validate your experience and respect your choices (control), you repair the deep breach of trust caused by trauma, allowing you to rely on your own judgment and instincts again.
How do I maintain my healing and stability after therapy ends?
Maintaining your gains requires committing to a trauma-informed lifestyle, where self-care is viewed as a safety protocol.
- Boundary Vigilance: Consistently practicing the boundary-setting skills you learned is essential to prevent future relational wounds and breaches of control.
- Daily Grounding: Maintain a daily habit of mindfulness or grounding check-ins to keep your nervous system regulated and prevent hypervigilance from creeping back.
- Self-Compassion: Apply the same non-judgmental acceptance to yourself that your therapist modeled. If you have a temporary “slip” or intense emotional reaction, treat it as a survival reflex that needs attention and skill use, not a personal failure.
Do I still need trauma-specific therapy (like EMDR) after TIC concludes?
It depends on your goals and needs:
- If you went through a formal trauma processing phase (e.g., EMDR): The TIC framework likely provided the stabilization, and the conclusion means the processing work is finished.
- If you only completed the stabilization phase: The conclusion means you are now safe and stable enough to begin formal trauma processing. You may transition to a different therapist or continue with the same one for a time-limited, memory-focused treatment phase.
- If you and your therapist agree you don’t need formal processing: You can conclude entirely, focusing on using your skills for daily life challenges.
People also ask
Q: What is trauma-informed healing?
A: Trauma-informed care (TIC) is an approach based on a foundation of knowledge about trauma and the paths to treatment, a response based on that knowledge and a desire to avoid re-traumatization, according to SAMHSA. Mars Girolimon.
Q:What is the definition of healing from trauma?
A: The guiding principles of trauma recovery are the restoration of safety and empowerment. Recovery does not necessarily mean complete freedom from post traumatic affects but generally it is the ability to live in the present without being overwhelmed by the thoughts and feelings of the past.
Q: What is healing informed care?
A: Healing-informed care is care based on Indigenous wisdom about wellness and what is necessary to heal. Culture has been shown to be a protective factor for AI/AN youth.
Q:What are the 5 stages of trauma healing?
A: The 5 stages of healing from trauma include establishing safety and stability, managing symptoms of PTSD, processing the traumatic memory, disconnecting from the trauma narrative, and achieving post traumatic growth.
NOTICE TO USERS
MindBodyToday is not intended to be a substitute for professional advice, diagnosis, medical treatment, or therapy. Always seek the advice of your physician or qualified mental health provider with any questions you may have regarding any mental health symptom or medical condition. Never disregard professional psychological or medical advice nor delay in seeking professional advice or treatment because of something you have read on MindBodyToday.
Share this article

Let us know about your needs

Quickly reach the right healthcare Pro

Message health care pros and get the help you need.
Popular Healthcare Professionals Near You
You might also like
What is Psychodynamic Therapy Principles?
, What is Psychodynamic Therapy Principles? Everything you need to know Find a Pro Digging Deeper: A Simple Guide to […]
What is Dialectical Behavior Therapy (DBT)?
, What is Dialectical Behavior Therapy (DBT) ? Everything you need to know Find a Pro Navigating the Storm: Understanding […]
What is Cognitive Behavioral Therapy (CBT)?
, What is Cognitive Behavioral Therapy (CBT) ? Everything you need to know Find a Pro Your Thoughts Are Not […]





